What is Maternal Health?
Maternal health is usually regarded as health during pregnancy, childbirth, and the period afterward. In other words, it is delimited by a time period and a physiologic state – parturition. Supporting maternal health is what every mother counts. It refers to a woman’s general health when she conceives and posts giving birth. Maternal health should not be confused with midwives, doctors, hospitals, trained birth attendants, and clinics. They are a part of it but not the only factors that define maternal health.
Health conditions or problems during pregnancy
During pregnancy, the body of a woman undergoes a great deal. Sometimes the changes in the body cause discomfort and irritation, and sometimes you have to be concerned. It would be best to mention everything that is bothering you during your pregnancy despite not facing any alarm.
There are many health conditions and problems during pregnancy that a woman has to face. Some of them are:
1. Constipation
You may become constipated due to hormonal changes that your body faces at the early stages of your pregnancy. Eat foods like cereals, wholemeal bread, vegetables and fruits, beans, lentils to avoid constipation. You may also exercise regularly to tone the muscles and drink plenty of water to prevent constipation. Try to avoid iron supplements and ask your doctor if there is an alternative. Iron supplements cause constipation.
2. Cramps
Sharp and sudden pain in the feet or calf muscles is known as cramps. Cramps are most common during the night time. There is no reason for cramps, but few ideas are about why they are caused and why it is faced during pregnancy.
You may exercise regularly during pregnancy, particularly leg and ankle movements, to prevent yourself from cramps. This will help to improve circulation.
3. Feeling faint
Often pregnant women feel faint. This happens due to changes in the hormone. Your brain is unable to get enough blood; hence there is not enough oxygen in the brain. This causes feeling faint when you stand up or are out of a bath. It may also happen when you are lying on the back.
There are many ways by which you can avoid feeling faint. Try to stand up slowly after lying or sitting down. In case you feel faint when you are standing, quickly find a seat and notice the feeling of faint is passing. And in case you are lying on your back and having the same feeling, turn on the other side. Try to avoid lying flat on the back during the days of pregnancy. It can result in higher chances of risk of stillbirth.
4. Feeling hot
You will experience a feeling of hotness during pregnancy again due to hormonal changes. The blood supply to the skin will increase, and you are most likely to sweat most of the time. Try to wear loose-fitting clothes that are made of fibers. Natural fibers are breathable and absorbent when compared to synthetic fibers. You must also keep your living room cool by using an electric fan. Wash frequently so that you can feel fresh.
5. Incontinence
This is a widespread problem faced by women during pregnancy. A sudden need to pee or small urine leakage cannot be prevented during pregnancy, usually, when they laugh, flick, cough while getting up from a sitting position, or sneeze. This is a temporary problem because the muscles around the bladder relax for the preparation of the baby’s delivery. Incontinence is treatable. Talk to your doctor regarding this issue.
6. Peeing a lot
During the early stages of pregnancy or in many cases until the baby is born, peeing a lot continues. This is mainly caused due to the head of the baby, which is pressing the bladder. To avoid this, do not consume drinks in the late evenings to get up to pee at night can be prevented. Try to consume a fair amount of non-alcoholic beverages and drinks free from caffeine during the daytime.
7. Hair and skin changes
Due to hormonal changes in the body, the nipples and the surrounding areas of the nipples will be darker. The color of the skin may also get darker, and there may be few patches. In case you have moles, freckles, and birthmarks, they may even get darkened.
There can also be dark lines below the middle of your stomach. These changes are temporary and will gradually fade once the baby is born. Try to protect the skin by using high-factor sunscreen and not expose yourself to the sun for a long time.
The growth of hair increases during the time of pregnancy. And the hair will be greasier. After the newborn, mothers complain of losing hair, but they shed off the extra hair.
8. Varicose veins
These are the veins that have swollen and are known as Varicose veins. They are uncomfortable but not at all harmful. Long veins are affected by varicose veins. Varicose veins can also be found at the vulva or vaginal opening. These problems become better after the birth of a child.
General Ask
Pregnancy complications
Before pregnancy
During the early months of pregnancy, you will need to pay more attention to some symptoms. You will face little bleeding, nausea, and vaginal discharge.
During pregnancy
There are most situations where pregnancies occur without any complications. However, there are also some complications faced by pregnant women, which makes their health and the baby’s heath complicated. But all these complications are for a short time and can be overcome easily.
Maternal health care
Before pregnancy
There are various steps you must remember to make yourself ready for the healthiest pregnancy possible. Some of them are:
Increase your folic acid – Folic acids help to make new cells in the body. During pregnancy, the cells are dividing at the same time, growing at a rapid speed. Folic acid is essential during the time of pregnancy. Folic acids can prevent anencephaly and neural tube defects. These occur during the early stages of pregnancy.
Preconception checkup schedule – It is imperative to get control of any chronic conditions when you are pregnant. Identifying the issues at an early stage can help prevent any disease and increase the chances of a healthy pregnancy.
Try to avoid drinking alcohol and restrict yourself from smoking – Drinking alcohol and smoking increases the chances of preterm delivery, SIDs or sudden infant death syndrome, NTDs, and fetal alcohol spectrum disorders. If you decide to stop such practices, talk to experts. Having support from the experts can help you to quit such practices very quickly.
Do not be overweight or underweight – In the case of overweight, the chances of facing difficulty in conceiving also increase. The risks of specific issues also increase rapidly during pregnancy. Try to shed the excess weight before becoming pregnant to avoid gestational diabetes, high blood pressure, and having a stillbirth.
Avoid certain fish – Certain fishes contain mercury. Try to avoid those fishes that contain mercury, such as shark, swordfish, king mackerel, and tilefish. Exposure to methyl mercury can damage the developing fetus. Consuming these fishes regularly will make your bloodstream full of mercury.
During pregnancy
Eat right
Get your vitamins
Try to stay hydrated
Certain foods must be avoided
Need for proper parental care is essential
Stop drinking alcohol
Get moving
Stop smoking
Get adequate sleep
Flu shot is important
Choose the best time to conceive
Do not take the stress
Avoid caffeine
Do light exercises, especially yoga
Get an adequate amount of iron and calcium.
After pregnancy
The period after the pregnancy is known as the postpartum period. This period is generally referred to as the first six weeks after the newborn. This period is a joyous and exciting time for the entire family. But for mothers, this is a period of healing and adjustments.
All these weeks, you will get a chance to bond with your newborn, and you will also undergo a post-delivery checkup. Follow these tips to keep yourself healthy during the postpartum period.
Get yourself plenty of rest
Try to seek help
Consume healthy meals
Exercise daily
The above mentioned are the common tips given to every mother during the postpartum period. But some mothers often undergo depression during this period. This is when the newborn is an adjustment for the mother and the entire family. A newborn can also change the dynamics with your partner.
Being patient is very important for starters. Every couple faces charges after a newborn, but it takes time and effort to overcome the changes. With each passing day, caring becomes easier.
You may sometimes face depression also. Try to communicate with your doctor in case you feel that depression is lasting for a longer time. The depression can develop any time after the delivery and is very easy to overcome by taking help from experts.
The bottom line
DELIVERY
What is Delivery/labor?
The delivery or labour of a child is the birth. This is the final stage of pregnancy in which the baby or babies emerge from the uterus. It is delivered either vaginally or via Caesarean section. Many major health organisations have recommended that as soon as a baby is born, whether vaginally or via C-section, the infant be placed on the mother’s chest.
This allows the mother and newborn to have skin-to-skin contact. Let us read more about delivery to get a better understanding.
Types of delivery for pregnancy
Bringing a baby into the world is a difficult task, but with proper planning and care, the task can be made much easier. Vaginal delivery is one of the most common and normal methods of giving birth. However, couples may look for other procedures and therapies that will make the task much easier, more convenient, and safer for both the child and the mother.
The following are some of the techniques that doctors and mothers prefer for a simple procedure.
- Vaginal delivery
Babies are frequently delivered using the womb’s birth canal as a support. This is referred to as natural birth or vaginal delivery. Most doctors will recommend this procedure if it is feasible.
When a woman plans to have multiple children, doctors will advise her to have vaginal births. If the incision is made above the anal, the procedure is known as an episiotomy.
- Cesarean section deliver (C-section)
In this type of delivery, an incision is made in the mother’s uterus or belly, and the baby is delivered through the incision. This procedure is now preferred by many women. As a result, C-sections make the delivery process much easier and safer for both the mother and the baby.
- Assisted Vaginal Delivery
The most common method of delivery is vaginal delivery. Doctors frequently use assisted type delivery when necessary. Labor is a simple and straightforward process, but it may occasionally necessitate the assistance of additional personnel.
The assistance is not limited to just delivery. It ranges from emergency delivery procedures to the use of specific medications.
- Water delivery
In the case of water delivery, the mother goes through all or some of the procedures associated with childbirth in a tub that resembles a hot tub. When the woman is under water, the baby is delivered.
A mother prefers different positions. This procedure is much more relaxing and avoids excruciating pain.
- Lamaze Technique
This method is a natural childbirth process that is popular for the controlled breathing technique it provides. This technique provides a variety of comfort strategies during delivery or labour.
The breathing technique it allows promotes relaxation and reduces the likelihood of pain. This method, in addition to the breathing technique, provides other techniques for preparing for childbirth.
- Bradley method
This method focuses on preparing a mother to choose natural childbirth with the help of her partner. They prepare for the procedure of unassisted vaginal birth without the assistance of medications.
This method is taught for twelve weeks with the help of family and friends, using workbooks to keep track of progress.
- hypnosis
This is a philosophical technique. This method teaches relaxation through breathing techniques, visualisations, and self-hypnosis. It induces relaxation, which is critical for the mother in a fearful situation.
This method fosters the potential of a woman’s faith in her body. During labour, the natural birthing instincts are activated. It helps to ensure a comfortable calm and serene birth.
The stages of delivery
Every woman’s labour is unique in its own way, beginning with the first pregnancy and progressing through the subsequent ones. Often, the process of delivery or labour takes an hour, and in some cases, labour puts a mother’s emotional and physical stamina to the test.
Nobody knows how childbirth and labour will go until it happens. The sequence of events will assist you in preparing for the same. There are various stages of labour and delivery. The following are the stages:
1. First stage
The start of labour is included in the first stage of labour. The cervix has been completely dilated. And the first stage is divided into three sub-stages once more.
Early labor– This is the shortest and least intense phase of delivery. This is also referred to as the latent phase of delivery. During this stage, the cervix is thinned and dilated to 3-4 cm. It usually takes days or weeks, but it can also take a few hours.
During this stage, contraction can range from moderate to severe, occurring at regular or irregular intervals. Mothers may experience symptoms such as bloody mucus discharge, backache, and cramps during this stage.
At this point, the majority of women choose to go to the hospital. However, many women will arrive at the birthing centre or hospital while still in the early stages of labour.
Active labor– As the cervix dilates to 7 cm from 3-4 cm, the next phase is seen, followed by the first stage of delivery. There are more intense contractions, as well as symptoms such as backache.
Transitional labor–This is the most intense phase of delivery, with the sharpest increase in contractions. They are stronger during this phase and reappear every few minutes, or every 60 to 90 seconds on average. The cervix dilates the last 3 cm in a matter of seconds.
2. Second stage
Delivery–During this stage, the cervix dilates completely. Some would-be mothers want to push right away or as soon as the cervix is fully dilated. However, there are some cases where the baby remains high in the pelvis.
3. Third stage
The delivery of the placenta occurs after the baby is born. Mild contractions will separate the placenta from the uterine wall, and it will move downwards towards the vagina. After the placenta is delivered, an episiotomy, or the process of stitching to repair a surgical cut or tear, will be performed.
4. Fourth stage
Recovery– Once the baby is born, the placenta delivers, and you and your partner will experience unimaginable joy, fatigue, and relief. Most babies require breastfeeding as soon as they are born.
Some babies also have to wait a long time. Doctors always advise breastfeeding a child as soon as they are born. The uterus will contract as soon as the new mother begins nursing. It will also reduce the amount of bleeding.
What happens after the delivery?
It is very vital for a mother to get preparation for the changes in the body post-delivery. Here is a list of things that a mother have expectations to experience after the delivery:
- In the first week, you will lose weight
- Enlargement of breasts
- Contraction of uterus
- Bruised and swollen vagina
- The expectation of vaginal bleeding
- Emotional mood
- Saggy stomach
- Dull hair
- Give attention to the pelvic floor
- Look after the stitches in case of C-section delivery
Risks involved in a delivery
There are certain risks that have an association with a child’s delivery. Doctors work from the very first day to reduce the chances of risks during delivery. Some of the risks are:
- Low birth weight
- Deficiency in nutrition
- High blood pressure
- Diabetes
- Multiple-birth pregnancies
Signs of delivery for a pregnant woman
In case you experience any of the signs and symptoms, be sure that it is time for delivering a baby:
- Lightning or when the baby drops
- Urge to urinate increases
- Passing of the bloody mucus plug
- Dilated cervix
- Effacement of the cervix
- Back pain
- Contractions
- A sudden burst of excitement and energy
- Diarrhea
- Water breaking- which is not the same as urination
- Joints are looser
- Gaining weight has restriction so as losing weight
Relief of pain in labor
Labor or delivery can be painful so it is better to know the ways that can help you to get relief from the pain. Here is a list of tips that can help you to overcome pain during labor:
- Massage
- Water therapy
- Breathing
- Moving around
- Relaxation
- Epidural
- Entonox- oxygen and nitrous oxide mixture
- Use of TENS machine
What to expect during a delivery?
A woman has to face many changes during the time of delivery. The muscles that are located at the top end of the uterus press down the bottom of the baby. The head of the baby further presses the cervix that also releases the love hormone known as oxytocin and brings on contraction as well.
Normal Delivery

What is a Normal Delivery?
Giving birth to a child is one of life’s most beautiful experiences. It will live on in your memory for the rest of your life. This is a completely natural method of delivering a baby by the expectant mother without the use of any medications or invasive methods. Before opting for a normal delivery, the expectant mother and her family must understand its goal. The expectant mother’s psychological and physical health is preserved during a normal delivery. The process of normal delivery or labour begins between 37 and 42 weeks of pregnancy.
When is normal childbirth recommended?
Normal delivery is always recommended for young, healthy women. They can go through this procedure with ease. Normal blood pressure, foetal position, and an active lifestyle are all indicators of a normal delivery. Here is a list of situations in which standard delivery is advised:
- When there is a strong desire to urinate as a result of the pressure exerted by the baby’s head as it presses the pelvic region and squeezes the bladder
- Between weeks thirty and thirty-four, the foetus shifts to a head-down or cephalic position, indicating that it is ready for delivery. When an ultrasound is performed, it indicates that the baby’s position has already shifted downward.
- Vaginal discharge will increase and is expected to be pink or white in colour, as well as occasionally stained with blood. These are the symptoms of a healthy pregnancy.
- Breasts will sore, which is also a sign of a normal childbirth.The breasts will feel uncomfortable and heavy when you will be in the final stage.
- The foetus begins to put pressure on the lower back, causing pain in that area. The foetus is actually positioning itself to achieve a head-down or cephalic position.
- Due to the upset bowel movement, expectant mothers may experience discomfort and cramping. This is as a result of increased hormonal activity.
- The water bag can sometimes break before the labour begins. Normal delivery is advised at that time. This breaking of the water bag is expected to happen during labour.
Stages of normal vaginal delivery
Normal delivery consists of four stages.
1) First stage-
This stage is marked by cervix effacement and dilation. The contraction thins the cervix, allowing it to open. This is referred to as effacement and dilation. As soon as the cervix dilates, the opening will be measured in centimetres by the doctors.
The cervix will widen by about 10 centimetres during the first stage. This widening lasts approximately twelve to thirteen hours for the first baby and seven to eight hours for the second baby.
The first stage of normal delivery also has three sub-stages. The following are the sub-stages:
Early labor–The cervix widens by four centimetres during early labour. The majority of the early labour days will be spent at home. It will be recommended that you continue your sexual activities. Doctors will advise you to rest, relax, eat light meals, drink clear fluids, and record your contractions.
Contractions may disappear with a change in activities, but as time passes, they become stronger. Expect to be in active labour when you can clearly distinguish between how strong, how long, and how frequent the contractions are, and when you will be unable to talk during the contractions.
Active labor–The cervix opens from four to seven centimetres at this stage. This is the time to go to the hospital. When you have contractions every three to four minutes and these contractions last for about sixty seconds, your cervix will open faster.
As labour progresses, the water bag eventually ruptures, causing a large amount of fluid to spill. Contractions also accelerate when the water bag ruptures. During this time, easy breathing is beneficial. Doctors also recommend focusing on relaxing and positive music or images, which have been shown to be beneficial.
To expedite your labour, you can also change positions, apply cold or hot compresses, massage, walk, sit upright, or stand. Relaxing in between and during contractions saves energy. This also aids in the opening of the cervix. Many hospitals use soaking tubs or whirlpools to relax patients and prevent discomfort.
- Transition
The cervix opens from seven to ten centimetres at this stage. This is one of the most difficult and painful parts of a woman’s labour. This is the stage at which the cervix fully opens. The contractions last sixty to ninety seconds and repeat every two to three minutes.
The intensity of the contractions will overwhelm you, and you will have very little time to rest. You might feel irritated, tired, frustrated, shaky, sick to your stomach, sweaty, and cold at times.
Slow breathing will help you at this stage, but uneven breathing patterns may also help.
2) Second stage-
The baby usually emerges from the birth canal. This is the stage in which the cervix is completely open and ends when the baby is born. The baby is brought down by contractions and intense pressure, much like a bowel movement.
Doctors may advise you to push through the contractions. The contractions will give you time to rest. The majority of the women are irritated and want to be alone at this time. This stage will continue until the baby is born.
3) Third stage-
This is the afterbirth stage. The baby is born, and the uterus continues to contract until the placenta pushes out. A placenta takes five to fifteen minutes to emerge after the baby is born.
4) Fourth stage-
This is the stage of recovery. When the baby is born and the placenta is delivered, the mother and partner will experience exhaustion, joy, and relief. Most babies require nursing within a short period of time after birth, while others may require more time. Doctors strongly advise mothers to breastfeed their children.
As soon as the new mother begins nursing her newborn, the uterus contracts. When nursing begins, the amount of bleeding will also begin to decrease.
Benefits of vaginal delivery
When giving birth to a child via normal delivery, the natural process of labour is followed. There are numerous reasons why this method of birth is superior to others. Among the reasons are:
- Healthier for the baby and the mother
The mother and child form their first bond in the first few minutes they are together. The infant’s bond with the outside world begins at this age as well.
The comfort provided by the mother’s voice and arm reassures the child of his or her safety. The child is placed in the arms of the mother during the natural birth process, and bonding begins from there.
- Lactation is stimulated
Natural hormones stimulate the natural process of birthing during labour and birth. During this time, endorphins, oxytocin, adrenaline, prolactin, and noradrenaline are secreted. The mothering hormone is prolactin.
- Protective bacteria is ingested from the birth canal
During pregnancy, the vaginal microbes change. The bacteria ingested by the child from the mother’s birth canal aids in the development of the immune system. This also improves the child’s digestion of solid foods and milk.
The human microbiota is formed during the birth process. It gives the vaginal microbiome an important role in the development process.
- Postnatal recovery is faster
This method of birthing allows the mother to recover much more quickly. There is no medical intervention involved. The body does its job and takes its time getting back on track.
Infections are more likely in the case of other techniques. Unnatural body interventions take a long time to repair. Because normal delivery protects the body from surgery, the risks associated with the use of a knife can also be avoided.
- Makes one confident
After giving birth naturally, the mother feels a sense of accomplishment and confidence. This sensation cannot be compared to anything else.
- Hospital stay is shorter
When compared to other techniques, normal delivery results in a much shorter hospital stay. It can last anywhere from twenty-four to forty-eight hours.
Symptoms of normal delivery
There are many symptoms of a normal delivery. Some of the symptoms are:
- Dropping of the baby
- Desire to urinate
- Lower backache
- Vaginal discharge increased
- Diarrhea
- The thin cervix
- Dilate Cervix
- Water bag breaks
- Sore breasts
Risks of normal vaginal delivery
Even if you are not having your first child, it is obvious that you will experience pain during the delivery process. Even if you have previous experience delivering a baby, you will have no idea how bad the pain can be during labour or how you will cope with the pain.
Despite the use of medications, every delivery carries some of the other risks. Some of the risks include problems with the umbilical cord or significant blood loss. These issues are extremely difficult to detect, and once identified, they require medication intervention.
Is natural birth painful?
Yes, childbirth is excruciatingly painful. If you want a normal delivery and your circumstances allow it, you will be able to feel every type of sensation. Normal delivery is one that does not involve any pain medication. Pressure and pain are the two sensations experienced during natural birth.
When the time comes to push, you will be relieved of some pressure. When the baby enters the birth canal, you will feel constant and increasing pressure during the contractions. As the baby descends and presses on a few nerves, you will experience an immediate bowel movement.
If doctors perform an epidural, the sensation you will have will be highly dependent on the effectiveness of the epidural block. You will be unable to feel anything if your nerves are rendered dead by medications. You will feel pressure if your nerves are only moderately effective.
The postpartum care after normal delivery
After a normal delivery, a woman can expect to experience postpartum bleeding for the next six weeks. The bleeding will feel like a heavy period. It is made up of tissue, blood from the uterus, and mucus. The bleeding will be at its peak for the first ten days, then gradually decrease, and the colour will shift from red to pink, then brown to yellowish-white.
Some of the tips are:
- Applying ice frequently for the first twenty-four hours after the infant’s birth will help the perineum heal faster. Warm water must be applied to the area after and before urination to properly clean the area and prevent irritation caused by urine.
- A warm sitz bath can help alleviate pain. Long periods of sitting, sleeping, or standing should be avoided.
- To relieve aches and pains, take paracetamol. A heating pad and hot showers can help prevent aches and pains. You could also get a good massage.
- The first postpartum bowel movement may take some time. Keep it simple and consistent. Take walks, eat lots of fiber-rich foods like fruits, whole grains, and vegetables, avoid straining, and use gentle stool softeners.
- Kegel exercises for postpartum women are essential. Begin exercising as soon as possible. It may assist you in getting your vagina in shape and making sex with your partner more enjoyable. The Kegel exercise can also help with postpartum urinary incontinence.
- Your breasts must be treated with care. Achy breasts can be relieved with ice packs, gentle massage, or a warm compress. A nursing bra is always beneficial for aching breasts. Crack nipples should also be treated with lanolin cream.
- Keep your doctor’s appointment. Your doctor will assist you in recovering from everything. If necessary, your doctor will also assist you in emotionally adjusting.
- Eating well can help prevent constipation and fatigue. Five smaller meals per day are ideal. A combination of protein, carbohydrates, and fibre is required.
- Throughout the day, drink plenty of water.
Your checklist for postpartum recovery are:
- Maxi pads
- Acetaminophen
- Witch hazel pads
- Ice packs
- Squirt or peri bottle
- Sitz bath
- Nursing pads
- Lanolin
- Cotton underpants
- Heating pad
- Nursing bras
- Stool softener
- Lidocaine spray
- Postpartum recovery belt
The recovery period after normal delivery
The first six weeks of postpartum recovery are crucial. Your body is stressed and stretched to the limit, and it requires some time to recover. Every new mother is unique, and their recovery period and postpartum symptoms vary as well.
The majority of postpartum symptoms resolve within a week, but some, such as backaches, nipples, and perineal pain, may take weeks to resolve. Some issues, such as back pain and leaky breasts, may persist for a longer period of time.
Depending on the extent of the episiotomy or perineal tear, the recovery time can range from three to six weeks. The vagina of a woman who has had a normal vaginal delivery is likely to be similar to but not identical to the older vagina.
When and how to push a baby out?
When the baby is born, you are about to complete the procedure. However, getting to that point may take some time. In the case of a normal vaginal delivery, some careful pushing is also required.
When the cervix has dilated completely, it is time for you to assist your baby in coming out by pushing gently. This could take anywhere from thirty minutes to an hour. However, the timing may differ from case to case.
Here are some tips for pushing;
- You must push just the way you do in bowel movements
- Your chin must tuck to your chest
- Give your maximum effort
- Do not lose focus
- Change your position
- Have trust in your instincts
- Take some rest between the contractions
- Stop pushing when instructed
- Keep your eyes on the mirror
How long does a normal delivery last?
Normal delivery times range from thirty minutes to one hour. It may also take a few minutes to finish the process. The timing varies according to the case.
Cost of normal delivery
The cost of a normal delivery may range between Rs. 15,000 to Rs. 20,000. Normal vaginal delivery along with epidural may cost n between Rs. 20,000 to Rs. 30,000.
Cesarean Delivery

What is Cesarean Section?
C-section delivery, also known as Cesarean delivery, is a surgical procedure used to deliver a baby through incisions in the lower abdomen. Couples prefer caesarean delivery because it allows them to choose the date of their child’s birth. There are no major risks associated with caesarean delivery. With this procedure, one can go through the experience of giving birth to a child without feeling any pain. Before deciding on a procedure, both parents must be aware of its benefits and drawbacks.
Why a cesarean delivery is done? (scheduled/unplanned)
Many women request C-sections when having their first child. It aids in the avoidance of labour as well as many other potential complications associated with vaginal birth. Because it is a planned delivery, this type of delivery also helps to obtain many benefits.
Both the baby and the mother are safer with a C-section or Cesarean delivery. A caesarean delivery may be recommended by medical professionals if:
- If the work does not progress: A stalled labour is one of the reasons for a caesarean delivery. It could happen if the cervix is unable to open sufficiently despite several hours of strong contractions.
- When the baby is in pain: If a baby’s heartbeat changes, the healthcare professionals will be concerned. Cesarean delivery is the best option at that time.
- When the child or children are not in a normal position: If the baby’s buttocks or feet enter the breech or birth canal at that time, caesarean delivery is the safest and best way to deliver a baby. Sometimes the baby will be in a shoulder or side fast position.That time also doctors perform a C-section delivery.
- A woman may carry multiples: A caesarean pregnancy is required when the woman is carrying twins and the baby who is leading is not in a proper position. This also occurs when a woman has triplets or more children.
- There may be a problem with the placenta, such as a cover at the placenta previa or an opening of the cervix. Doctors recommend a C-section delivery in that case.
- If the umbilical cord slips through the cervix ahead of the baby, doctors will perform a C-section.
- When there is a medical emergency: Cesarean delivery is also performed when there is a serious medical emergency, such as a brain or heart condition. A C-section delivery is required if there is an active genital herpes infection.
- Mechanical obstruction: A woman may require an emergency caesarean delivery if she has large fibroids that obstruct the birth canal or if she has a pelvic fracture. It is also when the baby has conditions that can lead to severe hydrocephalus, such as a larger-than-normal head.
- Women may have had a previous caesarean delivery. In that case, doctors may advise attempting VBAC, depending on the type of uterine incision and a variety of other factors.
Risks and complications of a cesarean delivery
There are many risks and complications that come with a C-section delivery. Some of the risks are:
- The majority of babies born via c-section have breathing difficulties, which is known as transient tachypnea. It is a type of breathing problem that begins with rapid breathing during the first few days after birth.
- Babies can sometimes be born through unintentional skin nicks. This is something that can happen during surgery.
- Women who have a c-section have a higher risk of developing endometriosis, which is an infection of the uterine lining.
- The infant’s large size
- Obesity
- Diabetes
How to prepare for a cesarean delivery
If you decide on a caesarean delivery, you must obtain all delivery instructions from your doctor. You must be well-versed in all aspects of risk reduction in order to avoid complications and have a successful delivery.
Not only c-section delivery, but all types of delivery require numerous checkups. Several blood tests and physical examinations will be performed during the prenatal appointments. It will aid in determining the health of the would-be mother in order to determine whether or not there is any risk underlying.
Your blood type will be recorded by your doctor in case a blood transfusion is required during surgery. It is extremely rare for a blood transfusion to be required during a caesarean delivery. Your doctor is always prepared for any complications that may arise during the delivery.
Even if a caesarean delivery is not planned, you must always be prepared for the unexpected. Always discuss the risks and complications, as well as what you can do to ensure a successful delivery. Make certain that all of your questions have answers.
When compared to vaginal birth, caesarean delivery always requires more time to recover. It is always a good idea to have an extra set of hands on hand. With help around you, you will recover quickly, and your baby will receive the care he or she requires.
The C-Section Procedure: What to Expect
What happens during a C-section?
It varies depending on the reason for undergoing the procedure. A c-section entails a number of steps. However, many things happen during the C-section.
You will be asked to shower with antiseptic soap the night before your delivery as well as the morning of your delivery. You will request that the pubic hair not be shaved because shaving within 24 hours increases the risk of a surgical site infection. Before the delivery, the surgical staff will trim the pubic hair with a trimmer.
Doctors will clean your abdomen and place a catheter in it. The catheter will be inserted into the bladder to collect urine. The doctor will also insert IV or intravenous lines into the patient’s arm or hand to deliver medication or fluids as needed.
There are three types of anaesthesia used during the delivery of a baby via c-section. The majority of caesarean deliveries are performed under regional anaesthesia. It aids in the numbing of the lower body by allowing the mother to remain awake during the delivery procedure.
In an emergency, doctors may opt for general anaesthesia. During the procedure, the mother will be unable to feel, see, or hear anything. An epidural block or a spinal block are two common types of anaesthesia.
The medicated doctors will make an incision above the pubic hairline once the patient is properly numb. In most cases, the incision is horizontal across the pelvis, but in an emergency, it is often vertical. Once the incision into the abdomen is made, the uterus is exposed.
Throughout the surgery, doctors will cover the area, so the patient will not be able to see the procedure. After the second incision, the baby will be removed from the uterus by the doctors.
It will then be cleared through the mouth and nose, and the umbilical cord will be clamped and cut. The baby will be given to the staff, who will monitor the baby’s breathing pattern. The uterus will be repaired with dissolving stitches, and the abdominal incision will be closed with sutures.
What happens after a C-section?
You will be admitted to the hospital for a few days following the caesarean delivery. The doctors will go over all of your pain relief options with you. You must drink plenty of water and walk around as soon as the anaesthesia wears off.
Deep vein thrombosis and constipation are both avoided. The doctors will also keep an eye on the incision site for signs of infection. The bladder catheter will also be removed shortly after the delivery by doctors.
You will be able to start breastfeeding your child at this point. You can also ask the nurse for advice on how to breast-feed a child and how to position yourself so that neither you nor your child is uncomfortable. To reduce post-surgical pain, you must be on medications.
Before the doctor orders you to go home, ask the doctors for advice on any preventive measures you should take. Make sure all of your questions are answered so you don’t have any problems at home.
Recovery and Care after a cesarean delivery
Giving birth to a child is the most exciting time of one’s life. After a nine-month wait, you finally get to meet your baby. The baby was growing inside you for nine months. Having a baby inside you can also cause some health issues.
More care is required when having a caesarean delivery. When compared to vaginal delivery, you will need more time to recover. Here are some suggestions that may assist you in hastening your recovery:
- Plenty of rest
Because caesarean delivery is a major surgery, your body will require more time to recover. You will be in the hospital for four to five days, or even longer if complications arise. A doctor will request six weeks from you in order to completely heal your body.
This is much easier to say than it is to do in practise. When your newborn baby is demanding your attention, almost everyone finds it difficult to crawl into bed for hours. When your baby falls asleep, you must rest.
Even a few hours of rest throughout the day can be beneficial. As for a helping hand to change diapers and do all household chores for your baby so you can rest, that is something you should consider.
- Take care of your body
Take extra precautions to protect your body while travelling. When climbing the stairs, try to avoid going down and up. Keep everything in front of your hand so you don’t have to go around too much. Try not to get up too frequently.
Nothing heavier than your baby should be lifted. Request assistance from a friend, domestic help, or your spouse. Try to hold your abdomen while coughing or sneezing to keep the incision site from opening.
It will take nearly eight weeks to get back to normal. Inquire with your doctor about when it is safe to resume exercising or driving. Avoid having sex until your doctor gives you the all-clear.
Avoid strenuous exercises in favour of gentle walks as much as possible. Your movements will assist your body in preventing and healing from blood clots and constipation. Walking will help your baby adjust to his or her new surroundings.
Remember to take care of your mental health as well as your physical health. When you have a baby, you will experience a wide range of emotions. When you are exhausted, disappointed, or sad, do not ignore your feelings. Discuss your feelings with your friends or family. Do not be afraid to seek professional assistance.
- Relieve your pain
Consult your doctor about which medications are appropriate for relieving pain while breastfeeding. Doctors will prescribe medications based on the level of anxiety and discomfort. Doctors may also recommend pain relievers such as acetaminophen or ibuprofen. Heating pads can also be used to relieve pain.
- Try to have good nutrition
It is critical for new mothers to consume nutritious foods. This is just as critical as good nutrition was when the baby was growing inside you. If you are breastfeeding your child, you are the primary source of nutrition.
Eating nutritious foods will keep you stronger and your baby healthy. According to studies, eating a variety of vegetables will result in different flavours in your breast milk. These flavours will aid your child’s consumption and enjoyment of these foods as they grow.
Remember to drink plenty of water and other fluids. Consuming extra fluids will increase your breastmilk supply while also preventing constipation.
- Walk regularly
For the first few days of recovery, avoid strenuous exercise. As a result, you can substitute walking for exercises. It can help you maintain good mental health as well as physical fitness. Walking reduces the risk of blood vessel or heart problems, as well as blood clots.
- Keep a record for signs of infection
Every 24 hours, you must keep track of your body temperature in order to monitor for infections. Other symptoms to be on the lookout for include intense pain, swelling, chills, and red streaks.
Benefits of cesarean delivery
There are many benefits of c-section delivery. But there are many chances of reducing the risk with c-section delivery. Some of them are:
- During and after giving birth the risk of pain reduces
- Lower chances of heavy bleeding post-birth
- Reduced chances of injury
- No loss of bladder control
- Low chances of pelvic organ prolapse.
Cesarean delivery cost
The average cost of a c-section delivery cost in India ranges from Rs. 50,000 to Rs. 2,00,000. This cost is without any medication and pre and post-surgery tests.
Painless Delivery
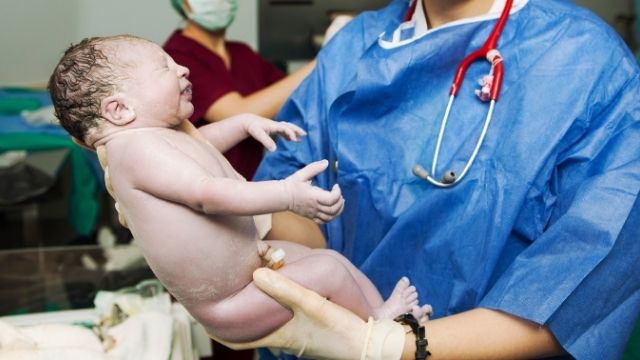
What is Painless Delivery?
Being a mother is a wonderful experience. However, a woman experiences excruciating pain during childbirth. When most women are pregnant for the first time, the pain becomes unbearable. However, thanks to revolutionary advancements, women now have the option of choosing painless methods. Painless delivery is a method that can help to reduce pain during childbirth while also allowing women to enjoy it. An epidural is a type of anaesthesia used to relieve pain during labour. After learning about the benefits of this procedure, many women prefer it.
What is an epidural?
An epidural is a type of anaesthesia used to relieve pain during labour. If you choose an epidural, a needle and a small tube called a catheter will be inserted into your lower back. In addition, the needle is removed and the catheter is left in place to deliver medications through the tube.
Doctors can administer epidural anaesthesia at any time during labour. It requires a physician consultation and can be given at the start, middle, or end of the treatment.
Only the epidural can be administered at any time once you are in active labour. It works by numbing the pelvic region and the lower portion below it while you are still conscious. You should be aware that this procedure does not guarantee complete pain relief.
How does an epidural work?
The timing of the epidural is critical. Doctors may prescribe an epidural immediately after a contraction begins or later as the labour progresses. Doctors generally prefer epidurals once the would-be mother is in active labour. Active labour occurs when the contractions are much stronger and closer together.
It may appear that having a needle inserted and a catheter inserted in the lower back is a painful procedure. Doctors will administer local anaesthesia prior to the procedure to alleviate pain. Once the epidural is inserted into the area outside the spinal cord, you will be unable to feel pain.
The epidural will allow you to move and push, but it is entirely dependent on the medication. You may not always be able to walk the entire distance. As the labour progresses, you will be able to feel the contractions but not the pain.
Painless delivery procedure
Drips will be helpful for fluids into the arms before the procedure begins. You can bend forward, sit up over a pillow, or even lie on your side. This will make it easier for the doctors to insert the needles correctly. Doctors will instruct you to remain still.
Doctors will clean your lower back with cold antiseptic. They will also inject a small amount of local anaesthetic into the skin of your lower back. Furthermore, the needle will be inserted between the bones of your spine, in the space surrounding your spinal cord.
Once the contraction stops, the anesthesiologist will insert an epidural needle. It is critical that the anaesthetist knows when you are having a contraction. Once the small soft plastic tube has been inserted, the needle will be removed by the doctor. The anaesthetic will be delivered through that tube and will eventually numb the pain.
Within five to thirty minutes, you will be pain-free. The epidural is most beneficial during the first stage of labour, but it can be administered at any time.
Who should have this procedure?
An epidural is available to all women who are in labour and require pain relief. This is not for people who have abnormal blood tests or are taking blood thinners. It is not necessary for you to have an epidural to have a normal delivery. The epidural can provide significant benefits in reducing labour pain.
There are some patients where an epidural is recommended to improve outcomes. Examples include:
- In the event that the woman’s labour is prolonged or complicated. It will benefit both the woman and the baby in this case. There should be no problems with a normal, painless, and stress-free delivery.
- If you are attempting a vaginal birth after a c-section (VBAC).
- If you have a medical condition like preeclampsia, heart disease, or hypertension.
Options for painless delivery
Having a baby is one of the most difficult things a woman must go through. Getting through the pain is a difficult task. However, doctors always advise patients not to panic. There are several approaches that can help you manage your pain.
Every woman is different in her ability to tolerate and experience pain. Doctors advise focused breathing to help you get through labour. However, some women require pain relievers. Here are some painless alternatives:
- Many non-pharmacological methods, such as hydrotherapy, hypnosis, and acupuncture techniques, can aid in painless delivery.
- Drugs are used in some pharmacological methods. Epidural analgesia, Entonox gas inhalation, and injecting epidural and opioids are some of the pharmacological methods.
Epidural analgesia (EA)
This is the most effective and dependable method of relieving labour pain. Local anaesthetic drugs will be administered into the epidural space using small tubes. It also aids in blood pressure control.
Entonox inhalation
A facemask is usually used to administer this mixture of 50% oxygen and 50% nitrous oxide. Inhalation must begin as soon as the contraction begins, so that its effect is maximised during the highest level of contraction. This is readily available and does not remain in the body for an extended period of time.
Opioid injections
This is the most common type of pain reliever for labour. Doctors normally inject this into a woman’s muscles, particularly her thighs. Each injection takes approximately 15 minutes. This painkiller’s effect lasts for a maximum of six hours.
Who should avoid It?
Some women should avoid epidural. Such as:
- Women who have certain bleeding disorders
- If someone is having lower back surgeries
- In case of neurological disorders
Painless delivery – Advantages and Disadvantages (Pros & Cons)
There are many advantages of epidurals. They are:
- Very safe
- Effective
- In the case of a long labor, the woman can sleep because of epidural and also recover strength
- It will allow you to move around in the bed and push whenever required
- It allows you to stay awake during the c-section procedure
The disadvantages of epidural are:
- Everyone cannot opt for this because of certain medical reasons
- Lose feeling in the legs for hours
Painless delivery side effects (Temporary & Rare)
There are some temporary side effects of epidural. Some of them are:
- Although epidurals are completely safe for both the baby and the mother, they can cause side effects such as breathing difficulties, fever, back pain, nausea, shivering, and dizziness.
- Mothers may also suffer from severe migraines as a result of epidural leakage into the spine.
- Numbness throughout the lower body.
Painless delivery cost
The cost of painless delivery may range between Rs. 5,000 to Rs. 10,000. The charges may vary depending upon the hospital.
Forceps Delivery
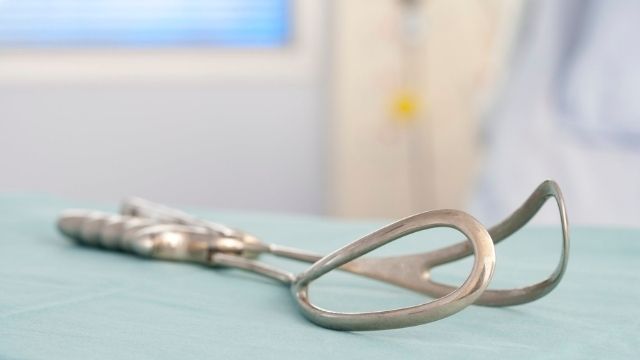
What is Forceps Delivery?
Forceps delivery is a type of assisted delivery. During labour, doctors use a pair of forceps. They are two large tongs used to guide the baby’s head through the birth canal. Doctors decide to use these tongs during labour to expedite the process. Forceps are typically used during vaginal childbirth during contractions while the mother continues to push. The use of forceps during delivery is uncommon in our country, but it is important to understand the details of this delivery.
When and Why is a forceps delivery done?
When pushing is involved, a forceps delivery is usually performed. When the baby reaches the midpoint of the mother’s birth canal, he or she is in the pushing phase.
Sometimes a baby has to struggle a lot to get out of his mother’s womb while labour is prolonged. As a result, the doctor decides to use tongs or forceps to expedite the delivery. Doctors may also use forceps during delivery to avoid a caesarean section.
Doctors may recommend forceps if:
- When the baby becomes entangled in the mother’s birth canal
- When there is a problem while pushing the baby, the forceps make things easier for the mothers. This usually occurs when the mother is exhausted or has a heart condition or high blood pressure. These conditions generally impede pushing and endanger the mother’s health.
- When the baby must be delivered quickly because the baby is experiencing foetal distress.
- When the baby’s position is unfavourable during the pushing stage. The use of forceps aids in the rotation of the baby’s head.
- Sometimes there is an issue with the baby’s heartbeat. Doctors at the time decide to use forceps to deliver the baby.
- When the position of the baby’s head is unknown
- The strength of the bones is sometimes determined by the baby’s condition. For example, the baby may have osteogenesis imperfecta or a bleeding disorder such as haemophilia.
- Because of the size of your pelvis, the baby may have difficulty fitting through.
How is forceps delivery performed?
The procedure involves:
- Two or more of the doctors’ fingers are inserted inside the vagina. The baby’s fingers are just beside his head.
- A portion of the forceps is slid between the doctor’s fingers and the baby’s head. The tong is slid by following the opposite side of the baby’s head.
- The tongs’ two parts are locked together to keep the baby’s head safe between them.
- During the mother’s contractions, the baby may occasionally face upwards. As a result, the doctors use tongs to shift the baby’s head into position.
- Doctors prefer to remove the forceps before the baby’s head enters the birth canal during the progression of labour.
- When the mother’s next contraction occurs, the doctor uses forceps to gently guide the baby through the birth canal.
Benefits of forceps delivery
There are many benefits of forceps delivery. Some of them are:
- Faster delivery
- The success rate of vaginal delivery with forceps is much higher.
- When these forceps are used, the chances of foetal scalp injuries such as subgaleal hematomas and cephalhematomas are greatly reduced.
- The fetal’s head can be rotated and correctly positioned using forceps, enhancing normal delivery.
- When used correctly during traction, the forceps do not detach from the fetal’s head.
- It is common to use general anaesthesia.
- Cord prolapse occurred during the second phase. They are a safer method when compared to caesarean or vacuum delivery.
Risks of forceps deliveries
Some of the risks are:
- Seizures
- Minor injuries in the face due to the extreme pressure by the forceps
- Some of the marks would be found on the face of the baby which is very normal for a forceps delivery and these marks are also temporary.
- Injuries in the urethra
- Urinary or fecal incontinence can be both long-term and short-term
Types of forceps deliveries
There are various types of forceps used in the assisted vaginal delivery or forceps delivery process. Some forceps are more commonly used in specific childbirth situations. As a result, hospitals prefer to keep a variety of forceps on hand.
Each forceps is ideal for specific situations, but when it comes to design, they are all the same. A forcep has two prongs and is useful for properly grasping the baby’s head. These prongs are the forceps’ blades.
The blades are variously sized curves. The right side blade is cephalic, while the left side blade is pelvic. The right blade is much deeper than the left. This is ideal for wrapping around the baby’s head, and the left side blade is shaped to fit against the mother’s birth canal.
Some forceps have a more rounded cephalic curve, while others have a more extended curve. The shape of the baby’s head is used to determine which forceps will be useful during delivery. A midpoint articulation exists where the two blades of a forceps cross.
The maximum forceps have a lock at the midpoint. The two blades slide due to the presence of sliding forceps. The baby’s position is also important in determining which forceps will be useful. Forceps with fix locks are useful when the baby’s head is facing downwards and there is little to no rotation required.
All forceps are made up of handles that are connected to the blades by stems. Longer forceps stems are useful when forceps rotation is required.
Types of forceps used for delivery
Some of the commonly used forceps are:
- Elliot forceps
They are made up of rounded cephalic curves and are frequently used when the baby’s head is round.
- Simpson forceps
They have extended cephalic curves and are common when the baby’s head is squeezed by the mother’s birth canal.
- Wrigley’s forceps
They are made up of short blades and stems that help to reduce the risk of a serious complication known as uterine rupture. This is most common when the babies are a long way down the mother’s birth canal. It is also common during c-section deliveries.
- Kielland forceps
A sliding lock and a shallow pelvic curve are used. They are most common when the baby needs to be rotated.
- Piper’s forceps
These forceps have downward curving stems that can fit around the underside of the baby’s body. During the delivery process, doctors usually grasp the baby’s head.
Forceps delivery technique
The techniques used for different forceps are:
Outlet forceps
- Without separating labia scalp at introitus
- Skull at the pelvic floor
- In AP diameter sagittal suture
- On the perineum, there is the fetal head
- Less than 45 degrees of rotation
Low forceps
- The skull is larger than +2 station
- Less than 45 degrees of rotation
- Greater than 45 degrees rotation
Mid forceps
- Head engaged, above +2 station
Forceps delivery indications
The indication for forceps delivery is both from the fetal and maternal side. None of the indications are absolute. Some of the indications of forceps delivery are:
- Engaged fetal head or vertex presentation
- Fully dilated cervix
- Membranes ruptured
- Knowledge about the position of the fetal
- The estimated weight of the feta
- Administration of anesthesia
- Adequate size of the maternal pelvis for a normal vaginal delivery
- Empty maternal bladder
- In case the operative delivery method fails, this is a backup plan
- Obtain consents when doctors will explain the benefits and risks are thoroughly
- Maternal neurologic and cardiac disease in case pushing is not advisable
What to expect with forceps deliveries
During the forceps delivery, you must lie on your back, incline yourself, and spread your legs apart. Doctors will instruct patients to grab the handles on the sides of the delivery table for support while pushing. During the contractions, the experts will insert two or more fingers inside the vagina and beside the baby’s head.
One of the forceps sections will gently slide between the baby’s hand and head. Another portion of the forceps will be placed on the opposite side of the baby’s head at the same time. The forceps will be locked together to support the baby’s head.
You must push while your health care provider uses forceps to gently guide your baby through the birth canal during the next contractions. In the event that the baby’s head is facing upwards, doctors will use forceps to rotate the baby’s head during contractions.
If the baby’s delivery is certain, doctors will remove the forceps by unlocking them before the widest portion of the baby’s head passes through the mother’s birth canal. Doctors prefer to leave the forceps in place so that the baby’s head can control the situation.
Doctors will examine the baby after the delivery to see if there are any tears caused by the use of forceps. Doctors will repair any tears that exist. Doctors will keep an eye on the baby for any signs of serious complications.
Recovery from a forceps delivery
If you are struggling after a forceps delivery, it is never too late to seek help. You’ll have a lot of questions about the delivery process. Consult your doctor for specific advice.
Do not be afraid to ask questions, as the nurses are happy to answer them. If you are still in pain, consult your doctor or a nurse. You will be given pain relievers on a regular basis to alleviate any discomfort caused by the stitches. For a few days, doctors will also prescribe anti-inflammatory drugs or paracetamol.
You must change the maternity pad as frequently as possible and wash your hands before and after doing so. A bath should be taken every day to keep your stitches clean. Notify your doctor if you discover any signs of infection. If you have difficulty urinating or notice bad odours from the stitches, you may have an infection.
As soon as you get home, the comfort of lying in bed will improve. This will assist in relieving pressure and pain. Squatting on the toilet rather than sitting will help to alleviate the stinging.
You can also choose to sit in a tub full of warm water so that the antiseptic in the tub can help to soothe the areas of the stitches and reduce swelling. At the same time, germs and infections will be kept at bay. The stitches must be dry in order to heal quickly.
If you have severe tears, your doctor will prescribe a liquid laxative to help you get rid of them. The laxative will have a gentle effect. You will also follow the recommendation to drink one to three litres of fluid and eat nutritious food.
To control your urination, try some pelvic floor exercises. Your baby may also have bruises as a result of the forceps delivery, but these are only temporary and will fade quickly. Your baby will not have any long-term problems as a result of the forceps delivery.
Vacuum Delivery

What is Vacuum Delivery?
When the mother’s labor is interrupted or the child’s health is a priority, a vacuum is used to perform a type of vaginal birth known as vacuum delivery. The doctor will use a suction cup with a pump to create suction if the baby has not moved in the past few hours. As the mother pushes, this will carefully guide the baby out of the birth canal. In addition to making a delivery that is both efficient and effective, this helps to reduce the risk of the baby being injured during a c-section.
Who needs a vacuum delivery?
It as a rule happens during the second phase of work when the cervix grows totally and the mother has been pushing for quite a while. Be that as it may, the method involved with pushing has no sufficient improvement. After that, the doctor might decide to use a vacuum to deliver the baby. A decrease in the baby’s heart rate may sometimes indicate fetal complications. To avoid serious harm to the baby, it will need to be delivered right away.
Vacuum conveyance is great for such a circumstance where specialists select to remove the child from the birth waterway quickly. Pushing can cause problems with some serious medical conditions.
Reasons for vacuum delivery
The cervix may tear and be injured if the cervix is not properly examined before proceeding with the procedure. Careful fix for cervix injury might prompt complexities in later pregnancies. Additionally, it occurs when the mother is exhausted due to prolonged labor. While the mother pushes on, the doctor may assist with a vacuum extractor to pull the baby.
The delivery is comfortable because of the team effort. When the baby’s head is in an abnormal position, the vacuum must be used to move it back to the correct position. Additionally, it aims to reduce maternal laceration.
When it’s done during delivery?
During the second phase of conveyance which is by and large the pushing stage, on the off chance that the child or the mother have openness to specific significant issues the specialist might utilize vacuum help extraction. Vacuum delivery is helpful in situations where the mother is pushing but not making much progress or is too exhausted.
One must ensure that the bladder is empty before going to it; evaluating the baby’s head position and maintaining sufficient anesthesia for assistance Vacuum conveyance is where extremely less sedation performs. Specialists forestall to the methodology of vacuum conveyance when the child doesn’t fit through the pelvis. Doctors may be unsure of the baby’s head’s position or the baby’s head has not progressed in the birth canal.
This procedure takes place only when the baby is sufficiently far down the canal, indicating that it is nearing birth. In the event that the head isn’t perfectly located specialists select cesarean birth.
How is vacuum delivery done?
The doctor may perform an episiotomy to widen the vaginal opening or administer an epidural to numb the pain at first. They decide to cut the muscle that runs from the anus to the vagina. He can likewise change the measurement of sedation to guarantee a more compelling pushing. The bladder should never be completely full.
The doctor will use the vacuum pumps to create suction during the contractions by placing the vacuum cups on the baby’s head in between contractions. During a contraction, this will prevent the baby’s head from entering the canal again and will direct the baby out of it. After the head of the baby exits the canal, the entire body is easy to deliver with a gentle push from the mother.
Indication of vacuum delivery
Risk and Complications of using vacuum
Frequently because of long work, the mother will in general get drained because of loss of energy. To continue with the delivery, this exhaustion sometimes necessitates external assistance. The baby’s rapid heartbeat is a sign that it requires immediate assistance from outside sources.
The mother’s previous health status can be cause for concern at times. This necessitates vacuum extraction to limit the mother’s time and energy. Pushing is risky because of conditions like high blood pressure, glaucoma, an aneurysm, and heart problems.
Extraction
Before deciding on a method of delivery, parents should be fully aware of this. Although this procedure also carries risks, vacuum delivery typically carries fewer risks. Risks that mothers face include
- Lack of control over urination or defecation Hematoma is a condition in which the vein and artery become injured. Vaginal pain and damage to the perineum
- damage to the genital region
Recovery after vacuum delivery
If an episiotomy is performed, recovery will take several weeks. The tear and wounds in the vagina could hurt at first before it gets better after certain weeks. It may take some time for severe wounds to heal. It is not uncommon to experience some discomfort during healing. One ought to counsel a specialist on the off chance that the torment deteriorates joined by fever or indication of contamination.
Pre Pregnancy Counseling

What is Prepregnancy Counseling?
Pregnancy counseling should be distinguished from antenatal care. Informed choice is a component of prenatal counseling that informs both men and women of the health issues that have the potential to interfere with pregnancy and conception. During this meeting, you and your accomplice will be urged to get ready for pregnancy and remain as sound as conceivable effectively. Additionally, the candidate will be optimized for managing any serious health issues. Couples who attend prenatal counseling are also made aware of the numerous rules and regulations they must adhere to during this time.
Why is it important?
Pregnancy counseling is not offered to every couple, but the counseling season is significant in most cases. A lot of the time, it turns out that a couple had a problem when they were trying to get pregnant, or that one of the partners has health problems that could make things worse. As a result, counseling can assist in resolving these problems.
The majority of issues that couples face during pregnancy can be avoided with counseling. Counseling before getting pregnant is important for a lot of different reasons. Reasons for this include:
- Counseling can assist the couple and the doctor in determining whether or not it is the right time to conceive.
- When couples meet with non-pregnant women or men, couples who go through pre-pregnancy counseling can understand why counseling is needed. As a result, they have the opportunity to receive advice regarding healthy lifestyle choices and wellness, which may ultimately result in improved obstetric and reproductive outcomes.
- Couples will have the opportunity to lower the likelihood of severe health effects on the fetus, mother, and unborn child.
- Any couple who decides to attend a counseling session should be told to get medical help before trying to conceive or as soon as they think they will be able to on time. The woman needs to be watched over on a regular basis to see if she has any medical issues.
- Diabetes, hypertension, and other medical conditions have direct effects on pregnancy. Couples will gain sufficient knowledge through prenatal counseling to seek expert assistance in order to manage the conditions optimally.
- Reviewing all prescription and non-prescription medications is part of prenatal counseling. This scanning process will help include nutritional supplements and herbal products that patients need because they affect pregnancy and reproduction but are not considered medications.
- Pregnancy counseling sessions include a presentation on screening pregnant women for identical genetic conditions. This is exceptionally lauded for ladies who are imagining.
- Women who are of reproductive age conduct an annual assessment of their vaccination status. It aids in the evaluation of the tetanus, diphtheria, and acellular pertussis toxoid, or Tdap; rubella-measles-mumps; Hepatitis B and varicella. The counseling session helps the patients get the flu shot every year. Women who are pregnant or are willing to become pregnant will be eligible for additional benefits as a result.
- The pre-pregnancy guiding meeting assists with surveying the necessity for STI or physically communicated disease screening.
- Patients will be asked about their drug, alcohol, and nicotine use during the sessions, so prenatal counseling is also necessary. The doctors will be able to evaluate the couple’s current medications and determine which ones are best for them with this information.
Who should go for it?
Pre-pregnancy counseling is a good option for anyone who wants to get the right advice and avoid any problems during and after the pregnancy. Candidates on this list ought to try these counseling sessions because they will undoubtedly gain a great deal from them.
- Competitors who have attempted over and over to imagine yet neglected to encounter the ideal results.
- Have previous records of miscarriages and stillbirths.
- when a previous child has congenital disabilities.
- Assume the couple goes through openness to ecological poisons. It could hinder the fetus’s growth during the first few weeks of pregnancy or interfere with the process of conception.
- On the off chance that the mother who is expecting experiences any way of life conditions like low pulse or hypertension, diabetes, and so forth.
- If either partner has a condition that affects the heart, liver, kidneys, or other organs.
- If the pregnant woman had a history of surgery that had an effect on her pregnancy, such as heart surgery or renal failure.
- In the event that the eager mother is experiencing immune system sicknesses.
What does pre-pregnancy counseling include?
Pre-pregnancy counseling includes educating the couple as well as the entire family about different aspects of pregnancy. Here is a list of services that pre-pregnancy counseling includes:
- Best timing of pregnancy
- Pregnancy spacing and family planning
- Psychiatric, medical, and surgical histories reviewed
- Current medications reviewed
- Genetic and family history reviewed
- Immunizations
- Screening of any infectious disease
- Assessing individuals with HIV or Human Immunodeficiency Virus
- Assessing of any use of the substance
- Exposure to sexual and reproductive coercion, violence, and intimate partner violence
- Assessing of any nutritional status
- Reaching and continuing a healthy body weight
- Assessment of daily exercise and physical activity
- Dating for pregnancy
- Chronic disease management
- Genetic carrier and disorder states
- Diabetes management
- Blood tests
What happens at a Pre-conception Counseling?
During prenatal counseling, a variety of assessments are carried out. The sessions’ happenings are listed below.
- Persistent sickness the board
Any lady having a serious sickness ought to survey that with the specialist at pre-origination guiding prior to getting pregnant. This might assist with decreasing the possibilities of dangers for both the kid and the mother.
- States of genetic disorders and carriers The genetic counselors are referred to families with a history of genetic orders during preconception counseling. The dangers of passing on the child’s disorders are discussed.
- Benefits of folic acid Counselors talk about how taking folic acid before or during pregnancy might help prevent neural tube defects (NTDs). During the meeting, ladies who are having the regenerative age are recommended folic acids. This is approached to be gone on during the pre-origination till the last day of pregnancy.
- Short-term pregnancies are characterized by high rates of maternal mortality, preterm birth, maternal morbidity, membrane rupture in the early stages, myometritis, anemia, and third-trimester bleeding.
The short-term negative effects of pregnancy will be diminished during the counseling session.
- Candidates for cessation of smoking will receive information about the use of tobacco during pregnancy and the days before conception. They’re all linked to low birth weight, preterm labor, placenta abruption, and intrauterine growth retardation.
Smoking cessation reduces infant mortality and low birth weight. Pre-origination advising assists the couple with picking smoking discontinuance. This will assist with decreasing the adverse consequence on the pre-birth period and richness.
- Consumption of alcoholic beverages The woman and her partner will receive information about the harmful effects of alcohol consumption during pregnancy. It is related with richness issues and fetal liquor disorder. There will be limitations on the utilization of liquor in the event that the couple is making arrangements for a pregnancy.
In the literature, there is no safe level of alcohol consumption during pregnancy. The result may be unfriendly neuropsychological results in the newborn child. Pregnancy counseling addresses this concern.
- Obesity is associated with diabetes, hypertension, congenital heart disease, and an increased likelihood of difficulties during pregnancy. Obesity-related complications can be avoided by taking the appropriate medications or consulting a dietitian, according to doctors.
- Underweight In order to lessen the likelihood that the woman will be deficient in nutrients, pre-conception counseling evaluates her for malnutrition. A lack of nutrients causes preterm birth and low birth weight.
- The executives of diabetes
During the pre-origination time frame, directing spotlights on instruction and illness the board, weight the executives, information about the normal dangers to the mother and the youngster, ideal control caused because of expanded degree of diabetes.
- Infectious disease management Couples receive accurate information regarding the mother’s and baby’s potential risks and treatment. There are various types of diseases that could make long haul antagonistic impacts. Infections like these are as follows:
- Hepatitis B
- HIV or Human Immunodeficiency Infection
- Lockjaw
- Measles, Mumps, Rubella, or MMR
Tests performed during preconception counseling
During the counseling session before getting pregnant, a number of tests are taken. A list of tests that were carried out is provided below:
- Blood tests on a regular basis are done to see how both partners’ health is doing. This test aids in determining whether the partners or individuals require any medication or treatment to avoid conception and pregnancy complications.
- CBC count The purpose of this test is to reduce the risk of anemia. Low hemoglobin has a negative impact on the health and development of the fetus.
- The pregnant woman is tested for antibodies to determine whether or not she is immune to German measles or rubella. On the off chance that she is viewed as not insusceptible, specialists recommend for inoculation. She shouldn’t get pregnant unless the virus is cleared from the blood, it is said. The ideal time is one month.
- Test for the thyroid The thyroid is a factor in infertility. In only a small percentage of cases does a test reveal the presence of thyroid. If a person decides to get pregnant without solving the problem, they might have a baby with a lower IQ and have trouble developing their brains.
- Screening for thalassemia This test is done on both parents to see if there is a thalassemia gene. The odds of having a child with this condition are 25%.
- Vitamin deficiency is a very common problem among women. However, deficiencies in vitamin B12 or vitamin D can harm a pregnant woman or a nursing infant. Correcting these problems during pregnancy or conception is essential.
- The purpose of the Pap smear test is to determine whether or not the cervix contains any cancerous cells.
- Genetic counseling This test can identify problems like stillbirth, recurrent miscarriages, restricted growth, congenital disabilities, and others if the couple had problems during a previous pregnancy. Treatments are given to lower or eliminate the chance of this happening again during the upcoming pregnancy.
- Physically sent illnesses tests
The two accomplices are tried for STI or physically sent infections like HIV, VDRL, Hepatitis C, and B.
How to get ready for the visit?
Always ensure that you and your partner are prepared before attending a prenatal counseling session. To get yourself ready, follow the suggestions below:
- If you have any records of a successful pregnancy, previous surgery, or medication use, you must keep them all in one place when you schedule a counseling session. Make sure that you both arrive with a list of medications and an individual’s medical records prepared.
- Be open-minded when you go to the chamber. Don’t always expect the doctor’s checkup and analysis to be in your favor. If things don’t go according to plan, don’t get discouraged. Attempt to search for additional choices and stop briefly to chat with your accomplice. Discuss the next action with your partner. The human body is unique, but significant advancements can resolve any issues that are discovered.
- Communicate effectively with your physician You must communicate effectively with your physician. Don’t forget to give the doctor any details. Before you decide to have a child, your doctor needs to know about any previous hospitalizations, vaccinations, and medications you both took. It’s possible that your prior history of substance abuse and health issues will prevent you from becoming pregnant at times.
What to expect during a Pre-pregnancy check-up?
What tAfter you and your partner have provided the doctor with your complete medical history, the doctor will begin the examination. Additionally, they will carry out a number of tests, such as a Pap smear and blood tests.
These tests are done to make sure that neither you nor your partner have any serious medical conditions that could affect how many days it takes to become pregnant or how likely it is that you will become pregnant.
You and your partner can benefit from taking a counseling test before getting pregnant. There are no negative aspects to the test. Numerous medical advancements can assist you in overcoming any issues discovered during the trial and delivering a healthy baby. Always make it a point to take this exam with an open mind.
High Risk Pregnancy

What is a High-Risk pregnancy?
A high-risk pregnancy is one in which either the mother or her unborn child’s life or health are in jeopardy. After some time, as they grow, some pregnancies can become high-risk ones. However, for a variety of reasons, some women have a history of complications. In cases like this one, it’s best to get help from experts or trained assistants. The chances of having a healthy pregnancy increase and the risks decrease when you receive proper care and regular prenatal exams.
Symptoms of High-Risk pregnancy
It is essential to pay attention to the body and remain alert at all times during pregnancy. To stay safe, keep an eye out for any signs or signals the body is giving you. The following are the signs and symptoms of a high-risk pregnancy:
- You are experiencing vaginal bleeding.
- The pain in the pelvis and the abdominal region is unbearable.
- You’re losing your mind. You should seek the assistance of others in this difficult circumstance.
- Your vaginal leak is present. The umbilical cord may be protruding into your vagina, causing this leak.
- There is predictable back torment or pelvic strain.
- Your baby is either not moving at all or moving less than usual.
- Your hands, face, and feet are swelling, you have a severe headache, and your vision is blurry. Preeclampsia is indicated by these symptoms.
Risks factors for High-Risk pregnancy
A high-risk pregnancy is associated with a few risks, which are outlined below:
- Overweight or weight – High-risk pregnancy can cause stoutness, which prompts hypertension, gestational diabetes, toxemia, stillbirth, cesarean conveyance, and brain tube deserts. Additionally, the baby’s heavy weight increases the risk of heart disease, according to researchers.
- Problem with her health: The mother might be HIV-positive, have high blood pressure, or have diabetes.
- Multiple births: Twins or triplets significantly increase the risk of high-risk pregnancy. Preterm birth, preeclampsia, and premature labor are among the complications. Before the 37th week of gestation, more than ninety percent of multiple birth babies were born.
- The mother’s age: Preeclampsia and high blood pressure are more likely to occur in a high-risk pregnancy if the mother is younger or older than 35 years old.
Medical conditions that occur during pregnancy
The greater part of the pregnancy experiences no ailments. However, if there is a problem, it could be bad for both the mother and the baby. While discussing inconvenience, hardly any circumstances are common like the accompanying:
Hyperemesis Gravidarum: All pregnant women experience some form of morning sickness, but what happens if it gets worse a thousand times? The condition of HG is this severe illness. Women with HG experience severe nausea, necessitating either immediate hospitalization or sudden weight loss.
Gestational Diabetes: Macrosomia refers to the condition in which the baby’s growth is greater than usual. During labor, the baby’s shoulder may become stuck as it grows in size. The doctor may perform a cesarean section if the situation described above is not suitable for standard vaginal delivery.
Previal placenta: The placenta’s main job is to give the baby oxygen and nutrients it needs to grow properly. Normally, the placenta is on the highest point of the uterus. Be that as it may, for this situation, it is between the uterus and the vagina, i.e., the cervix. Extreme vaginal bleeding is the disease’s primary symptom.
Preeclampsia: Preeclampsia occurs when a woman has too high a blood pressure, which can be fatal. Preeclampsia can occur after twenty weeks of pregnancy. Preeclampsia can occur in women regardless of whether they have high blood pressure. Preeclampsia should be checked out by your doctor if you have vision problems, severe headaches, and back pain.
Management of High-Risk pregnancy
For managing a high-risk pregnancy, you can follow the following guidelines:
Know your problem: If you experience any abnormalities that could indicate a medical condition, you should always see a doctor. Different infections require prompt consideration, similar to development diabetes, toxemia, placenta previa, or fetal anomalies. In the event that you experience the ill effects of any of the accompanying, you should realize every one of the entanglements connecting with it to stay away from a conveyance issue.
- Inform your family and solicit the assistance of your partner and family. Inform them of the complications and explain them to them. During this time, you will require loved ones to communicate your sentiments and help you out working. They can also assist you if you suddenly fall unconscious. A high-risk pregnancy support group is another option. It is very helpful in maintaining optimism and building confidence.
- Take care of yourself: If you’re having a high-risk pregnancy, you should take better care of yourself and your baby. Eat a decent solid eating routine, have a decent rest, discharge your pressure, play out a light activity, and avoid hurtful climate. With standard delivery, these suggestions can be very helpful.
- Pay attention to your body – You should stand by listening to yourself, do anything that you want to do. If you feel like resting throughout the day, do so. If you feel like eating, do so. You can always alter your routine, so it’s not necessary to stick to it every day. Also, tell your doctor if you are not feeling well inside.
- Express your feelings: During pregnancy, you may experience a lot of emotional turmoil and mood swings. It is typical. Please do not conceal your feelings. Express it with all of your heart. Be at ease; Your loved ones will comprehend. Health-related stress or even hormonal changes can cause mood swings. Do some meditation if you have a lot of emotions; It will assist you. Take a walk or talk to a friend to distract yourself.
Do and Don’ts of High-Risk pregnancy
It’s a good idea to be familiar with all the rules. It makes the cycle a great deal simple and solid. Try to adhere to it for a healthy birth:
Dos:
- Before beginning your pregnancy planning, talk to your doctor about the right conditions for having a baby.
- Prenatal vitamins can be taken one to two months before you become pregnant with proper guidance from your doctor.
- Get regular exercise and eat a well-balanced diet.
- Go for ordinary tests during your pregnancy to check the wellbeing of your child as well.
- For a healthy delivery, you must always ensure that you deliver in the hospital with appropriate medical support.
Don’ts
- Don’t be afraid; It may have an impact on the baby’s health.
- Do not conduct online searches for health issues. All things considered, ask your primary care physician.
- Please do not take any medication after researching it online or asking a family member to see a doctor.
- Don’t eat too much when you think you can feed two people.
High-Risk pregnancy tests
Your doctor may perform certain high-risk pregnancy tests, such as:
- Amniocentesis is a procedure in which the doctor takes a sample of the patient’s amniotic fluid for testing. This test recognizes surrenders like Tay-Sachs, spina bifida, and hemophilia.
- Chorionic villus sampling is a procedure in which the doctor takes a sample of placenta tissue to look for conditions like Tay-Sachs, Down syndrome, and hemophilia.
- Blood cell samples and fetal anemia are tested during the doctor’s fetal heart failure checkup. To gather the test, the specialist gathers some blood from the child’s umbilical rope.
- Genetic testing is done by the doctor to look for conditions like cystic fibrosis or muscular dystrophy.
- During a high-risk pregnancy, an ultrasound test is very helpful. A routine ultrasound can tell if the baby has any problems. Doppler ultrasound can gauge the blood stream inside the child to guarantee its wellbeing.
Diagnosis in High-Risk pregnancies
Going for determination during and even before pregnancy is an ideal choice. It helps in forestalling any difficulties in pregnancy.
- You should get a targeted ultrasound while you are pregnant to rule out any potentially fatal diseases.
- Additionally, cell-free DNA screening during pregnancy aids in the detection of any potential chromosome issues. Both the mother’s and the child’s blood samples are examined.
- You can likewise quantify the size of the cervix through ultrasound to stay away from the gamble of preterm work.
- Lab tests related to urinary tract infections or infectious diseases like HIV and syphilis should be requested by your physician.
- You can also use the information from your prenatal ultrasound to create a biophysical profile of your baby. This ultrasound shows you information about your baby’s health and monitors the fetal heart rate.
Preventing and Testing pregnancy complications
Preventing all pregnancy-related complications is essential. So in the event that something is not exactly right, you ought to go for checking and play out the accompanying test:
- Check to see if there are fewer healthy red blood cells: this could result in anemia. Quickly treat the essential driver of iron deficiency for again reestablishing typical red platelet count.
- Go for testing urinary parcel disease for any contamination that could develop. In the event that you have a consuming sensation while peeing or strain in the lower paunch, your pee smells horrible, or queasiness, check for UTI.
- Have an unexpected weight gain or stoutness; could result in problems, so take steps to prevent them. Visit your physician for a consultation.
Twins or Triplets Pregnancy

What is Multiple Pregnancy?
Multiple pregnancies may occur if more than one egg fertilizes and grows in the uterus. Fraternal twinning is the birth of boys or girls with similar features in a large number of pregnancies. The placenta and amniotic sac of the babies are distinct.
However, in the case of identical twins, the egg fertilizes and divides into two, resulting in either a male or a female child. Although they may not share a single placenta, these identical twins have a distinct amniotic sac. They may share a single amniotic sac in some instances. Despite their similar appearance, these children have distinct personalities and are distinct from one another.
Management of multiple Pregnancies
If you take care of the following things, complications caused by multiple pregnancies can be controlled and managed:
- Food that is healthy: If you are carrying two or more children, you need to give them the right nutrients. In order to provide them with the necessary iron, protein, and other nutrients, the mother will need to consume more nutrients than usual. Weight gain is additionally fundamental in various pregnancies for standard conveyance.
- Visit the doctor more frequently: The doctor advises attending more prenatal appointments to prevent complications before they occur. Additionally, frequent visits guarantee that any potential future issues will not arise.
- Get enough rest and pay attention to your body; Give yourself a proper nap if you need more rest. Various pregnancies need more bed rest than expected.
- Tocolytic medications: Tocolytic medications can slow down contractions in preterm labor. These medications can be taken orally or injected.
- Cervical Cerclage: The woman’s cervix is weak and cannot close during pregnancy in this instance. So cerclage is performed to line the cervix opening.
Testing during pregnancy is essential for determining the health of the infant. It additionally assists with checking difficulties, if any.
How are multiple pregnancies delivered?
The following factors can affect the number of babies delivered:
- Gestational period and fetal positions Your health and the health of your baby.
- If both of the fetuses are positioned with their heads down, delivery will not be an issue; for this situation, standard vaginal conveyance is conceivable. However, if both are upside down and facing in opposite directions, use the vagina to give birth to the first one.
- The second one must either be delivered through the buttocks or moved to the vertex position. In this contrary heading case, difficulties might build, prompting playing out a crisis cesarean or C-segment.
- Most different conveyances is through C-segment. In cases of complications like fetal distress, specific health issues in the mother, and the fetus’s abnormal position, a C-section is recommended.
Early signs of multiple pregnancies
Each woman indicates different signs. However, most commons are:
- Extreme morning sickness
- The uterus is more extensive than usual for the particular month of pregnancy
- Greater appetite
- Excessive weight gain
- Movement of the fetus felt in different positions of the belly at the same time.
Symptoms of twins during pregnancy
There may be some symptoms that can indicate that you are carrying a twin:
The amount of hCG produced in the body is higher than usual as they are enormous for two fetuses.
You can hear the baby’s heartbeat from eight to ten weeks from a device called fetal Doppler. When you hear from the device, two heartbeats are hearable.
There is an abnormal increase in weight. Usually, upto twelve weeks of pregnancy, there is an increase in weight of 1-4 pounds in the women. But if you experience more, it’s a sign of multiple pregnancies.
Causes of multiple pregnancies
There can be a ton of variables that can cause numerous pregnancies. Some are as per the following:
- Age of the woman: Women over the age of 30 have a greater chance of having multiple pregnancies. They may conceive twins because they delayed the procedure.
- Heredity – In the event that there is a hereditary history of imagining a twin, the opportunity of numerous pregnancies increments.
- More births: You are more likely to have multiple pregnancies if you have been pregnant multiple times.
- Race: If you are American or African American, you are more likely to have multiple children. In addition, Asian and Native American women have the lowest odds of having twins.
Complications of multiple pregnancies
A twin or higher-standard pregnancy can result in a number of problems:
- Gestational Hypertension: Women who have multiple children are more likely to have high blood pressure. Hypertension can influence the child’s placenta, and it has a danger to get isolates from the suitable spot.
- Paleness – It is far and wide in numerous growths, which can increment difficulties during birth.
- Miscarriage: The vanishing twin syndrome is very common in multiple pregnancies. In this disorder, one of the hatchlings gets evaporated or prematurely delivered. There could be bleeding or not. Typically, miscarriage occurs during the first trimester.
Risk of multiple pregnancies
Both the mother and the unborn child face risk during a twin pregnancy. While carrying twins or triplets, the mother faces numerous threats. Hypertension, preeclampsia, gestational diabetes, premature labor, hyperemesis gravidarum, C-section, and numerous others are among these threats. While certain dangers are simply slight intricacies, some can cause genuine risk like fetal passing. Both the mother and the baby may be put in danger by these.
The gamble that is engaged with the child is the danger of getting disappeared. To put it another way, there is a possibility that one of the babies will be miscarried. There is also the possibility of having intrauterine growth discordance, in which one twin does not grow in the same way as the other. Twin birth can bring about underweight newborn children or the infants getting jaundice.
Types of multiple pregnancies
- Twin pregnancy
At the point when one single undeveloped organism partitions into two, it structures indistinguishable twins. The risk of this kind of pregnancy is lower than for identical twins. DNA is the same for each embryo because it contains the same genetic material. Because they share the same DNA, the twins will share the same traits but have different personalities. They have the same placenta and amniotic sac, but occasionally they have different ones.
There is one more sort of twin who is brought about by various eggs. They could be of the same gender or not. Although they share a uterus, their placenta and amniotic sacs are distinct. Fraternal twins are the name given to this kind of twin.
- Pregnancy with triplets can result in either fraternal or identical twins fusion. Development of trios happens from three separate treated eggs, or they can be indistinguishable, as framed from a solitary prepared egg that breaks into three, or a combination of both the condition.
Diagnosis of multiple pregnancies
If there are multiple pregnancies, you can make the following diagnosis to avoid any problems at delivery:
Testing for HCG: Your doctor can look for human chorionic gonadotrophin (hCG) in your blood.
Ultrasound – There should be a legitimate examination of the body’s inside to peruse its blood stream. For the purpose of creating an image of internal organs, blood vessels, and tissues, this check involves recording sound waves.
Alpha-Fetoprotein – In this test, estimation of how much protein discharged by the fetal liver. To avoid problems, the mother should keep the amount of protein released constant.
Prevention of multiple pregnancies
A brilliant choice to keep away from various pregnancies is to forestall some barrenness conditions. You can avoid multiple births if, as a precaution, you do not implant multiple embryos in the uterine walls.
A woman who has enlarged ovarian follicles or high hormone levels is more likely to have multiple children. Therefore, taking steps to stop an egg from fertilizing if it has more than three follicles can help lower the risk of high-order pregnancies.
In the event of triplets or a high-order pregnancy, multifetal pregnancy reduction can be performed to ensure a healthy delivery. However, the treatment carries the possibility of a complete miscarriage. Additionally, it may lower the risk of a premature birth.
Chromosomal disorders
What is a Chromosome Disorder?
Chromosomal disorders are any condition in which an abnormal number of chromosomes results from malfunctions or malformations in any of the body’s systems. Each pair of chromosomes is numbered in a specific order and has a variety of shapes and sizes. The remaining twenty-two pairs are autosomes, while the sex chromosomes make up one of the pairs. Assuming there is any divergence in the example, it causes irregularities. Any of the pairs may replicate or not have any chromosomes, and an unaffected set of twenty-three pairs of chromosomes may also replicate three or more times.
What is a chromosome test during pregnancy?
Chromosome testing is prescribed by specialists when specialists need to see the consequence of the hereditary tests. Your child’s medical condition will be better understood based on the results of this test. Every individual can have a changed design of hereditary materials in the cells. The doctor can use this to determine whether the child has any abnormalities or not.
Amniocentesis and CVS, also known as chorionic villus sampling, are the two types of chromosomal testing.
The procedure known as amniocentesis involves removing the amniotic fluid from the uterus and sending it to a laboratory for further examination and treatment. During pregnancy, this fluid is responsible for surrounding and safeguarding the baby. Different kinds of proteins and fetal cells are present in the amniotic fluid. Using amniotic fluid, important information about the baby’s health can be gathered. Amniocentesis can assist with deciding:
Testing of the fetus’s lungs This fluid can help determine the condition of the baby’s lungs and whether or not they are ready for birth when it is taken out of the uterus and tested.
Genetic testing involves testing the fluid that is taken from the uterus to identify conditions such as Down syndrome.
Paternity testing
Amniocentesis assists with gathering DNA that can measure up to the DNA of the possible dad.
Treatment The aim of treatment is to remove the excess amniotic fluid from the mother’s uterus so that the fluid does not interfere with pregnancy.
The diagnosis of a fetal infection is helpful in determining whether the baby is ill or infected. The diagnosis process continues based on that.
One of the prenatal tests, chorionic villus sampling (CVS), involves removing the chorionic villi from the placenta for examination. Either the cervix or the abdominal wall are used to collect the sample. The placenta is in charge of removing waste products from the blood and providing oxygen and nutrients to the developing infant. This test should be possible as soon as 11 to 14 weeks of pregnancy.
Any chromosomal condition, such as Down syndrome or any other genetic disorder, such as cystic fibrosis, can be identified through this test. This test provides useful information regarding the baby’s health. You should likewise be ready to comprehend the dangers implied and plan for the results of the test.
When the outcomes from the pre-birth screening test are positive?
When the results of the screening tests, such as prenatal cell-free DNA screening or first-trimester screening, are problematic or positive, your doctor may recommend this test, or you may choose to take this sampling test. It assists with deciding if there is any requirement for determination or not.
Have you ever had a previous pregnancy with a chromosomal condition?
Once in a while the past pregnancy is impacted by some chromosomal condition or down disorder. As a result, the risk of the current pregnancy may also be higher. This test is suggested by the doctor to determine whether there is a risk.
- Suppose the woman is 35 years old or older.
- Women with down syndrome are more likely to conceive when they are 35 years old or older.
Is there a history of a genetic condition in the family, or is one of the partners known to be a carrier?
This test can assist with distinguishing on the off chance that the child is having down disorder or not. Additionally, it aids in determining whether the baby is affected by any underlying genetic conditions. This test can also identify single gene disorders like Tay-Sachs and cystic fibrosis.
When to see a doctor?
Doctors may recommend a chromosome test during pregnancy for the following reasons:
Abdominal pain that does not go away with rest or paracetamol Bleeding from the vagina Leaking of fluid from the vagina Feeling suddenly unwell with high temperatures
Risk factors for chromosomal disorders in pregnancy
Pregnancy-related risk factors for chromosomal disorders include:
- A history of multiple miscarriages or stillbirths The mother must be 35 or older, and the father must be 40 or older.
- Causes of chromosomal abnormalities in pregnancy
- Every cell in our body has a chromosome structure that looks like a stick. It is in the middle of each cell. There are 23 sets of chromosomes in each and 46 chromosomes. Anything that goes wrong with a chromosome affects the entire body.
An error during cell division can cause chromosomal abnormalities during pregnancy. Anomalies can occur for the following reasons:
Teratogens are things to which a mother is exposed during pregnancy, such as various medicines, alcohol, toxic chemicals, tobacco, radiations, bacteria and viruses, and uncontrolled diabetes. Meiosis is an error in the dividing of sex cells. Mitosis is an error found while diving other cells.
Symptoms of chromosomal abnormalities
Some of the symptoms of chromosome abnormalities are:
- Infertility
- Head shaped abnormally
- Little to no hair on the body
- Height of below average
- Muscle mass reduced
- Physical and mental impairments
- Very less birth weight
- Openings in the mouth or lip
- Disabilities in learning
- Defects in the kidneys, heart, stomach, lungs, and heart
- Distinctive features of the face
Prevention for chromosomal abnormalities during pregnancy
As you get older, your chances of passing on chromosomal abnormalities to your offspring rise. Preventing chromosomal abnormalities during pregnancy necessitates specific actions. The steps include:
- Counsel a specialist before 90 days you need to consider. Talk about your medical problems, history of your wellbeing, vaccinations, and medications
- Abstain from drinking liquor and smoking
- Take pre-birth nutrients consistently for a very long time before you need to consider. There should be 400 micrograms of folic acid in the medications.
- You should continue to visit the specialist frequently
- Attempt to devour quality food varieties. Essential are foods high in folic acid, such as grains, orange juice, peanuts, and breakfast cereals.
- Start the process when you are at a healthy weight. Only doctors who are aware of your pregnancy should give you drugs.
Types of disorders can be seen during the time of pregnancy
As you get older, your chances of passing on chromosomal abnormalities to your offspring rise. Preventing chromosomal abnormalities during pregnancy necessitates specific actions. The steps include:
- Counsel a specialist before 90 days you need to consider. Talk about your medical problems, history of your wellbeing, vaccinations, and medications
- Abstain from drinking liquor and smoking
- Take pre-birth nutrients consistently for a very long time before you need to consider. There should be 400 micrograms of folic acid in the medications.
- You should continue to visit the specialist frequently
- Attempt to devour quality food varieties. Essential are foods high in folic acid, such as grains, orange juice, peanuts, and breakfast cereals.
- Start the process when you are at a healthy weight. Only doctors who are aware of your pregnancy should give you drugs.
Testing for chromosomal disorders
There are two types of chromosomal disorders tests. These are:
- Diagnostic tests—These consist of multiple tests—help determine whether the baby has any genetic disorders. Screening tests This helps identify specific genetic diseases thanks to its findings.
- The tests for chromosomal issues are discretionary. As a result, women who don’t run any risk can get them.
Treatment for chromosomal disorders
Chromosomal disorders affect a person’s genetic makeup. Because of this, no treatment can bring them back. However, there are still some treatments that can assist those with chromosomal disorders in making their lives easier.
Physical or occupational therapy, growth hormone injections, and hormone replacement therapies are some of the treatments. These will assist in treating some of the symptoms and issues associated with chromosomal genetic disorders.
Double Marker Test
What is Double Marker Test?
Actually, the double marker test or dual marker test is a screening test for maternal serum. This test is done by doctors during the first trimester of pregnancy. Examining the amount of pregnancy-associated plasma protein and b-human chorionic gonadotropin (a pregnancy hormone) in erythrocytes is helpful.
This is recommended by doctors for women over the age of 35 because they run the risk of giving birth to a child with Down syndrome. The nuchal translucency (NT) is a dual marker test that can be used in conjunction with another test. It affirms the finding of any hereditary irregularities.
Advantages of double marker tes
- It aids in determining the trisomy of chromosome 13. It is to blame for the infant’s mental retardation and severe birth defects.
- Most importantly, finding the chromosomal aberration at position 21 that causes Down syndrome is helpful.
- It aids in the detection of pregnancy-related risk factors. It also aids in determining whether it would also be harmful to the mother’s health.
- If the mother tests positive for this abnormality, this test has a high detection rate, giving the couple time to evaluate the entire situation. Additionally, it is helpful to inquire about their willingness to undergo additional tests to verify the accuracy of the results. or whether they are pursuing MTP.
How to prepare for this Double Marker Test?
An ultrasound scan and a blood sample are used in this test by doctors. The machines and apparatus should be prepared for sterilization beforehand. Before the test begins, information about the patient’s weight, diabetes, and in vitro fertilization should be prepared for the maternal screen.
When is the test recommended?
If the woman who is pregnant is over the age of 35, this test is ideal. By looking at their pedigree chart, it can be determined if they exhibit any elevated signs of genetic aberrations.
Double marker test uses
To find out if a newborn has down’s syndrome and prevent it from happening, look for muscle loss, a short neck, and excessive skin growth at the back of the neck.
for the mother’s health and to prevent severe mental and physical handicaps, flattened faces, slanted eyes, and stunted growth in the newborns.
Determine the trisomy of chromosome 18, which would otherwise result in clenched fists and abnormalities of the heart, lungs, stomach, and intestines, as well as other vital organs necessary for the body’s proper metabolism and operation.
“Rocker bottom feet,” or feet that deform into the shape of a rocking chair’s bottom, can be used to identify a disorder.
Microcephaly, a small and deformed head, micrognathia, scrunched fists, an arched spine, and an abnormally shaped chest are all signs of microcephaly.
to find a short sternum and brain delays in neurological processes.
Recognize umbilical hernia in the event of the mother conveying the youngster.
How is this Double Marker Test Performed?
This test is very simple to perform since we just require the blood test of the pregnant mother. The subsequent steps include:
The blood sample is taken from the arteries with the help of a syringe.
The medical care supplier will then tie a flexible band on the arms consequently causing enlarging of the veins.
When the corridors are plainly noticeable, a sterile assists with clearing off the specific region under perception.
The inclusion of the needle happens finely into the vein with a pinprick. The example assortment happens first and protection occurs and afterward for testing.
This test carries no such risk. A female may experience increased bleeding, hematoma formation, bruising, or infection at the needle prick site in extremely rare instances.
How are the test results interpreted?
The aftereffect of the above test can fall under two classes – screen positive and screen negative. The test anyway doesn’t just rely upon the blood tests. The mother’s age and the child’s age are also important considerations. It likewise relies upon the timeframe when the test happens during the 9 months of the growth time frame utilizing a ultrasound.
The outcomes are in this way present in the reports as proportions. Screen positive results are those with a ratio between 1:10 and 1:250. They are exceptionally risky for both the mother and the creating undeveloped organisms.
A ratio of at least 1:1000 is a secure result with fewer threats or risks. A ratio of 1:10 indicates that one in ten pregnancies has a very high risk of developing a disease. Thus, a ratio of 1:1000 would indicate that one out of every 1,000 pregnancies has a development risk factor. This is very insignificant.
The doctor might recommend additional diagnostic procedures like amniocentesis in the event that the test results are positive. There is a good chance if the tests come back positive and the parents want to carry on with the pregnancy. That could also be the baby’s death during pregnancy.
Result of dual test normal range
For all age groups, the Free-beta Human Chorionic Gonadotropin range should be between 25,700 and 2,88,000 mIU per ml. This is the above-concerned test’s normal range.
Double marker test cost
The reputation of the institution affects how much the Dual marker test costs. It also depends on how accurate the test results are, how sensitive the instruments are, and what the machines need. Twofold marker test cost on a normal premise, Ranges fairly between Rs 2,500 to Rs 4,000.
Difference between double marker and triple marker test
The double marker and triple marker tests are identical and do not differ in any way. Triple marker tests are performed after 13 weeks, and double marker pregnancy occurs in the first 13 weeks. After a double marker, you don’t even need a triple marker, if your doctor says so.
Triple Marker Test
What is Triple Marker Pregnancy Test?
Between the 15th and 18th weeks of pregnancy, a triple marker pregnancy test is performed. Specialists at times prescribe the triple marker test to analyze in the event that there is any hereditary problem in winning the hatchling or not. It is known by a number of names, including AFP plus, triple test, multiple marker screening, and multiple marker test.
The levels of AFG (Alpha-fetoprotein), hCG (Human chorionic gonadotropin), and estriol in the blood are measured from blood samples taken from a pregnant woman. The results of this test let couples know if their baby is healthy or not.
Reason for the triple marker test
The results of this test reveal the fetus’s risk factors. It is used to look for congenital disabilities and neural tube defects like spina bifida and anencephaly. It is helpful to determine whether or not the fetus is at risk for Down syndrome. Down condition is a hereditary problem coming about because of strange cell division, in this manner delivering an additional duplicate of chromosome 21 in every phone.
The triple marker test can also be used to determine whether the pregnant woman is at risk for trisomy 18 (also known as Edward’s syndrome, which is a disorder in which each cell contains three pairs of chromosome 18 instead of two pairs) or whether she is expecting more than two children. Additionally, this test identifies all of the baby’s abnormalities.
How is the test performed?
Similar to other blood tests, the triple marker pregnancy test is easy to perform. The steps include:
Step 1: The technician will first ask you to extend your arm and make a fist, just like with any other test, to help him locate the vein.
Step 2: Second, this point will be securely held in place by a strap that will be wrapped around the arm.
Step 3: The technician will then disinfect the area with an antibacterial and antiseptic cloth to prevent pathogens from entering your body.
Step 4: Then, a pre-cleaned needle and another one will be embedded, connected to a vial utilized for blood capacity.
Step 5: The technician will use a second antiseptic and antibacterial swab to clean the area after the vial is full.
Step 6: A laboratory will receive the collected blood sample for evaluation. The selection will be evaluated by the lab’s biochemist.
Step 7: Software will store the results, which will then be sent to the doctor. From that point onward, the reports will be imparted by the specialist to the pregnant couple.
This test has not yet revealed any such adverse effects. Since how much blood removed is small, there is no possibility of critical blood misfortune from the body. As a result, both the mother and the baby are protected.
Alternative screening test
Couples may occasionally opt for a different screening test. In order to gain a deeper comprehension of the diagnosis, this is a second opinion on this case. A prenatal ultrasound can be beneficial. If you want to know which test to choose, it’s always best to talk to your primary care doctor about a list of other options. Additionally, you can select multiple advisors.
Precautions to take during the test
It is a lot of fundamental to unveil all your instructive data to the specialist while going through the test. The test’s results may change as a result of error. Specialists ought to continuously be cautious about attracting blood to guarantee that embryo isn’t impacted by any blood-borne microorganisms.
As a result, new needles and antiseptic and bacterial wipes should be used. There is no such firm guidelines for mother, yet specialists ought to follow it whenever recommended by specialists.
Benefits of triple marker screening test
A triple marker pregnancy test is exceptionally gainful for ladies who are over the age of 35. because there are fewer eggs in the ovary at this age. During her pregnancy, one might experience a lot of complexity. In spite of the fact that by this test, one can find the inherent handicaps in a child, subsequently assisting both the guardians with planning for a similar ahead of time.
A few hereditary issues or imperfections incorporate the accompanying:
A common type of chromosome abnormality is Edward’s syndrome, also known as trisomy 18.
A condition known as Down syndrome occurs when the cell contains additional genetic material from chromosome 21.
As previously mentioned, neural tube defects are birth defects affecting the entire nervous system, including the brain, spine, and spinal cord.
Who benefits from the triple marker test?
The majority of women over the age of 35 are recommended for the test by doctors. This test can also be beneficial to couples with a history of congenital disabilities. These test results may be satisfactory to diabetic women who take insulin. It assists with deciding if the child is impacted or not.
The triple marker test also helps people who have been exposed to a lot of radiation. Ladies having extreme viral contamination during pregnancy can likewise decide on this test however certainly with a specialist’s interview.
Interpretation of the test result
The fetus’s genetic disorders and other abnormalities are revealed by this test. However, the outcomes are subject to the following factors:
Age of women who are pregnant Women are born with a specific number of eggs. During each period, they continue to lose every one of them; as a result, they diminish as people age. Eggs present in more established ladies might have unusual chromosomes that can prompt hereditary problems.
Ethnicity There are certain ethnic groups with a higher birth rate than others. There are many variables answerable for such varieties the whole way across the world, for example,
This could be because of determinant of egg and sperm quality.
- lifestyle-related variation in environmental exposures.
- dietary elements.
- Cultural and socioeconomic factors.
- Fertility treatment accessibility
- Conduct towards looking for clinical consideration and subsequently, regenerative results.
- Body Mass Index (BMI) of the woman Regardless of whether she is expecting one or more children, an excessive BMI is harmful to both the mother and the fetus. Multiple pregnancies can result in complications. One needs to be much more mindful at this point.
Preparation of triple marker screening
There is no such readiness required for an imagining mother during a triple marker pregnancy test. Additionally, there are no such restrictions on food consumption. But a healthy diet is essential for both the mother and her unborn child during pregnancy. However, if you want the best advice, you should always talk to a trusted and experienced doctor.
The usual range of triple marker test
Pregnant women had an average of 1.38 to 187.00 IU/ml of AFP, 1.06 to 315 ng/ml of hCG, and 0.25 to 28.5 nmol/l of uE3 for the triple screen markers.
Results of a triple marker test
One will know whether the test report’s outcome is positive or negative after analyzing it. Negative screen results demonstrate that the embryo is extremely low or not in danger of fostering any inherent handicaps. If a doctor isn’t satisfied with the values, he or she may also order a lot of additional tests.
Triple marker test cost
The price of a triple marker pregnancy test can vary depending on a few things. The precision of the outcomes is directly correlated to the instrument’s sensitivity and the machine’s use. The institute from which the test will be administered also needs to be taken into consideration. By and large, the negligible reach is Rs.2,500, while the greatest sum might surpass Rs.4,000.
Quadruple Test
What is Quadruple Test?
A prenatal test is the quad screen or the quadruple marker test. It assists with recognizing regardless of whether there are any birth abandons in the child for instance conditions, for example, Down’s disorder, brain tube surrenders, trisomy 18 (Edward’s condition), and stomach wall absconds. A phlebotomist—a technician who specializes in drawing blood—collects the mother’s blood sample for evaluation. It is a basic interaction and there are no particular advances that expect to be followed. The woman is able to drink and eat normally. In the second trimester, the quadruple test is conducted.
Why the quadruple test is done?
If the pregnancy is likely to have certain conditions like Down’s syndrome, neural tube defects, trisomy 18, also known as Edward’s syndrome, or defects in the abdominal wall, this is the best method for evaluating the pregnancy. It should be sent for additional screening and testing if the test results show any of the conditions or results mentioned above.
Throughout the pregnancy, the levels of the aforementioned substances always fluctuate weekly. Knowing the stage and phase of pregnancy prior to stepping through this examination is dependably fundamental. Each biomarker is equipped for distinguishing specific irregularities in the child’s wellbeing.
For instance, if the Quad screen test reveals elevated levels of AFP in the blood, it indicates a neural condition like spina bifida. For another situation, in the event that the experimental outcomes show low degrees of AFP, the condition can be a Down’s disorder.
Women may receive advice to undergo prenatal tests in addition to the Quad screen test at times, depending on the timing of the pregnancy and other symptoms. Along with the quad screen test, some tests, like an ultrasound (USG) and a blood test, are recommended.
How the test is performed?
If the pregnancy is likely to have certain conditions like Down’s syndrome, neural tube defects, trisomy 18, also known as Edward’s syndrome, or defects in the abdominal wall, this is the best method for evaluating the pregnancy. It should be sent for additional screening and testing if the test results show any of the conditions or results mentioned above.
Throughout the pregnancy, the levels of the aforementioned substances always fluctuate weekly. Knowing the stage and phase of pregnancy prior to stepping through this examination is dependably fundamental. Each biomarker is equipped for distinguishing specific irregularities in the child’s wellbeing.
For instance, if the Quad screen test reveals elevated levels of AFP in the blood, it indicates a neural condition like spina bifida. For another situation, in the event that the experimental outcomes show low degrees of AFP, the condition can be a Down’s disorder.
Women may receive advice to undergo prenatal tests in addition to the Quad screen test at times, depending on the timing of the pregnancy and other symptoms. Along with the quad screen test, some tests, like an ultrasound (USG) and a blood test, are recommended.
Risks of quadruple test
This quadruple test reveals no such risk traces. On the other hand, this test is detested by many members of the family because it causes them anxiety. If it is determined that the baby is suffering from any conditions, abortions can be performed even in some instances without the mother’s consent.
Additionally, the mother is frequently to blame for the baby’s conditions, which frequently result in numerous serious issues. One thing that ought to be as a top priority is that after the blood test there can be blood trickling out from the injury. If it continues, you should see a doctor right away.
How do you prepare?
It is not necessary to physically prepare for the test; rather, discussing the potential outcomes should prepare one emotionally for the test. The following considerations must be kept in mind when preparing:
Timing: If the doctor deems it necessary, you can take the test as soon as possible at a clinic nearby.
Location: For the most part, doctors will send you to a clinic to take the test. You can find specific locations where these tests are performed from their annexure if you have a medical claim.
What to wear: Anyone can dress however they please and feel at ease. To ensure a smooth blood test, half sleeves should be preferred. Some of you could disapprove of the noticeable swathe after the test. As a result, one can carry any clothing to cover themselves.
Food and beverages: When it comes to food and beverages, there are no restrictions. Specialists frequently give suggestions to eat or drink something prior to getting your blood tests. It is so you will not be woozy thereafter.
What to Bring: Eat enough protein and drink enough water to avoid fainting. Even if it is warm outside, you should bring a jacket or a shawl because some people get cold after the blood is drawn.
Quadruple test results
It might require roughly seven days for your test results to be prepared. The four hormones under investigation are represented by numerical values in your quad screening test results. If you have access to your medical records and can sign in, you may be able to look up the test results on a computer. Your doctor will keep the results.
It’s possible that there won’t be any comments or assessments about your baby’s risk of certain conditions in the report itself. A doctor who is experienced in caring for pregnant women is needed to interpret these results.
The lab results and their meaning are as follows:
AFP: Anencephaly or spina bifida may be present in the developing child if your AFP is elevated above the normal range. A low AFP level may indicate Down syndrome.
Estriol: Estriol deficiency may indicate Down syndrome, anencephaly, or Edwards syndrome.
HCG: Anencephaly or Edwards syndrome have low HCG levels, while Down syndrome has elevated levels.
Inhibin A: With Down syndrome, high levels of inhibin A are found.
Elevated degrees of HCG are additionally assuming you are pregnant with more than one child. An evaluation of conditions and risks must take into account more than one of the four criteria. There is a possibility of either over or underestimating the risk of problems with the baby or the pregnancy when using the quad screen test.
Quadruple test cost
This test probably applies to your health plan in general. Additionally, there is a possibility that the expense will not be covered at all by your health plan. By calling the information number on your insurance card, you should be able to obtain information regarding your coverage and the cost. By giving them the name of the test, it is done.
The out-of-pocket cost of the test can vary greatly if you are paying for it yourself. It differs from laboratory to laboratory and even between regions. There is a reasonable specialist charge and an expense for handling. You can check the expense of the specialist charge with your primary care physician’s office or clinic.
In the event that you are required to pay a copay, you should also make sure to bring the test order, a form of identification, your insurance card, and a method of payment.
NIPT
What is Noninvasive Prenatal Testing?
The method for determining whether the fetus may have chromosomal disorders or genetic abnormalities is non-invasive prenatal testing, or NIPT. NIPT can see the high and generally safe of a hereditary condition. Because of this, it is not a diagnostic test but rather a screening one. When parts of a chromosome are missing or duplicated, the structure of the chromosome can change. NIPT incorporates evaluating for such extra chromosomal problems. Turner syndrome, Down syndrome, Edward syndrome, and patau syndrome are also identified by it.
What does NIPT test for?
NIPT basically searches for an extra or lost duplicate of the X and Y chromosomes known as sex chromosomes. It likewise distinguishes Edward condition (trisomy 18, which is brought about by an additional chromosome 18), patau disorder (trisomy 13 because of an extra chromosome 13). Furthermore, Down disorder (trisomy 21, which is brought about by an additional chromosome 21) can likewise get identified.
How is the NIPT done?
Any abnormalities can be identified with the help of a straightforward blood test using the mother’s blood. The report from the NIPT and the mother’s first-trimester ultrasound or nuchal translucency screening will be matched by the doctor. It will conclude regardless of whether there is any requirement for additional tests.
Indications for NIPT
NIPT should be taken by pregnant women at high risk. Women with a higher maternal age, such as those over the age of 35, a previous affected pregnancy, and unusual fetal ultrasound detection are considered to be at high risk. Another explanation is the point at which the serum screen report is positive, past private or family background of a hereditary problem.
How accurate is NIPT result?
Due to the fact that the condition affects less than one percent of all children who are born, the result is typically 99 percent accurate. A demonstrative test, for example, amniocentesis is tremendously prescribed alongside NIPT to have a precise outcome. When a condition is not present in the fetus, the NIPT issues a report with a high probability. NIPT is more accurate than standard screening tests.
Who it’s for and when it’s done?
NIPT is completed between 9-10 weeks of incubation to the furthest limit of the pregnancy. A few guardians choose standard screening at first and afterward choose to get a NIPT in the event that the customary screening report accompanies a high opportunity or positive rate. If blood has already been collected for NIPT, pursuing a conventional screening is not recommended. For Additional data about the child’s wellbeing, it is encouraged to take a nuchal clarity ultrasound in the first trisemister.
It typically applies to couples with a personal or family history of chromosomal deformities—women over 35 who are very mature when it comes to childbirth—or to women who are pregnant.
Steps involved in NIPT
In order to check for genetic disorders like Down syndrome, Edward syndrome, and patau syndrome, it looks at cell-free DNA from the mother’s blood sample, which is a combination of DNA from the mother and the fetus. Before all else, the plasma is isolated from the mother’s blood. The plasma’s cell-free DNA is then extracted and examined. Information is made from the formed sans cell DNA. The data are finally examined by advanced research.
NIPT is prescribed for high-risk moms presented to explicit issues that emerge the chance of having a youngster with hereditary deformations. A straightforward blood test can detect chromosomal abnormalities (if any) in a non-risky manner. The report is basically given an unmistakable “yes” and “no”, and it is conveyed inside a tiny time, which is beneficial as it ensures early treatment. Anxious mothers especially benefit greatly from it.
Since NIPT does not highlight certain genetic conditions, it is less reliable until other tests like CVS or amniocentesis are performed. When there are more than two fetuses in the womb, such as triplets or quadruplets, NIPT is not recommended. NIPT has been shown to cause termination in Down syndrome tendencies, which is a social issue that is gaining attention due to the growing impact of technology on our way of life.
Advantages of NIPT
NIPT’s gamble factor is lacking as the interaction contains just gathering a blood test from the mother. NIPT has gained notoriety for giving precise outcomes for maternal blood tests on high-hazard and okay pregnant ladies. Along with NIPT, amniocentesis is a highly recommended test for obtaining a precise result. Nonetheless, there is a possibility of miscarriage and it may not always be as accurate as it claims to be.
It quickly identifies genetic abnormalities. A quick response to chromosomal deformities typically takes 10 to 14 days. Typically, the report ends with a “yes” or “no.” Couples are much more likely to move forward if the information is delivered quickly.
NIPT test cost
A solitary trial of NIPT at first costs at Rs.50, 000 to Rs.60, 000 in India which is presently Rs.25,000. The underlying high pace of the tests is on the grounds that the specialists sent the examples to another country for assessment. This is because there aren’t many labs in India; however, some labs have begun conducting tests within the country. The price was lowered as a result.
OB-GYN Ultrasound

What is an OB-GYN Ultrasound?
High-frequency sound waves are used in OB-GYN ultrasound to image women’s internal organs. This makes it easier to look inside the uterus, bladder, cervix, fallopian tube, and ovaries of a woman. There are two reasons for using an OB-GYN ultrasound: at the hour of pregnancy, it screens the child’s wellbeing, and at the hour of regenerative issue. Uterine fibroids, ovarian cysts, and abnormal bleeding are all examples of this disorder. The inner parts are seen on a PC screen for the specialists to break down the circumstance. The procedure does not involve any discomfort.
What is ultrasound test?
It is a medical test that your doctor does to look inside your body to look for or analyze the disorder’s root cause. A live image of the body’s organs is displayed on a monitor using high-frequency sound waves in this situation. Sonography is another name for a test using ultrasound.
Since no radiation is used to capture the image, this method is also safe for monitoring the fetus. It assists with survey organs like the bladder, kidneys, eyes, cerebrum, ovaries, gallbladder, liver, and so forth.
You may need an Ultrasound at different phases of pregnancy:
- First and foremost, they are utilized to affirm regardless of whether the mother has considered.
- Second, knowing a lot about the baby, like its gender, position, and size, is helpful. In addition, if he or she is healthy or has a defect, it is used to determine whether twins or triplets are possible and when they will be born.
- Thirdly, it’s important to know if the baby is in the right position; is that they are facing the wrong way.
How to perform an OB-GYN ultrasound
You might be asked to lie on your side on the table by the doctor. However, in order to obtain a clearer image of the internal organ, the radiologist or sonographer may request that you turn to the side. The radiologist will then apply a gel-like liquid to your skin where the test will be performed. All air bubbles or gaps between the transducer and the skin are eliminated by this gel.
The transducer is rubbed into your skin in a circular motion by the doctor over the area you need to be examined. The procedure continues until the monitor displays the internal image. The movement of the transducer on the skin does not cause any pain; However, you may experience discomfort if it is a sensitive area.
What transpires?
-On the examination day: Prior to the test, you will need to drink a lot of water on the specified day; Up to three liters of water could be used. Eating anything before the stomach scan is fitting not. Most of the time, people show up in loose clothes to avoid having any trouble with the test. Additionally, some centers provide a gown that you must wear throughout the process.
-Throughout the exam: The doctor will apply gel to your abdomen while you lie down on the table during the procedure. He will utilize a transducer to play out the test, and you will see the picture of the inside organs on the screen. It will make the pictures as the specialist will focus on the transducer your skin. Usually, the exam is over in ten minutes.
You can use Ultrasound to perform the following procedures:
Assessing the location of the placenta and the fetus to determine whether or not there is a fetus.
- determining a child’s conception age.
- determining whether multiple births are possible.
- determining how much amniotic fluid is present around the baby.
- Assessing the shortening or opening of the cervix.
- determining any abnormalities in the fetus.
How should you prepare?
Hydrate before the cycle. When you come in for ultrasonography, always wear clothing that fits loosely. Additionally, since you will be required to expose your abdominal region during the procedure, wear a two-piece garment. Transvaginal ultrasound may be recommended by the sonographer or radiologist to confirm early pregnancy. You can get a closer and more in-depth look at the cervix and pregnancy with this kind of ultrasound.
What you can expect
Throughout the process: The ultrasound test is usually painless and takes little time. However, in order to obtain a clearer image or recording, the radiologist may need to press the transducer against the area. Although this may be uncomfortable, it will not be painful.
The Doppler gadget helps in the test. You will be able to hear the fetus’s blood flow. Additionally, the doctor may cause some discomfort when inserting the transducer into your vagina during a transvaginal ultrasound. However, don’t worry because the inserted transducer is smaller than usual.
After the strategy: At the point when the test is finished, you can spruce up, and you should sit in the lounge area for some time. You will receive the ultrasound images and test results after some time has passed. You can carry out your usual activities during the test.
What are the benefits vs risks?
The following are some of the test’s advantages:
- Because they don’t use a needle or an injection, you won’t feel any pain during the procedure.
- Ultrasound is a straightforward procedure that is less expensive than the majority of imaging techniques.
- The cycle is alright for the hatchling as it includes no radiation.
- It gives a more clear image of the inside region, which you don’t get in x-beams.
- It assists the specialist with seeing inside the belly and even lay out early pregnancy.
- There is no risk involved in the process. It does not in any way harm humans.
What are the limitations of obstetrical ultrasound imaging?
Obsetreical ultrasound imaging is limited in its ability to detect fetal anomalies. Therefore, in order to evaluate any disorder, if there is any possibility of fetal anomaly, you will need to choose a non-radiology test like an amniocentesis, blood test, or chorionic villus sampling. Additionally, you might need to see a perinatologist, who specializes in high-risk pregnancies.
Side effects from ultrasound
There are no dangers or result of the cycle up to this point. Dissimilar to CT examines, they don’t include radiation, which can make harm or mischief the baby.
Your internal organs will not be affected by the examination, and it will not be painful at all. There might be a sensation of discomfort in some places, but there is no actual pain.
However, in order for your radiologist to use a probe cover that does not contain latex, you must inform them immediately if you are allergic to latex. You might experience side effects like bloating or a sore throat if you don’t do this.
What happens after the pelvic ultrasound?
After your pelvic Ultrasound, you can return to your daily existence. Afterward, you are not required to alter your daily routine or schedule. You can still eat and drink normally. Follow the recommendations if the doctors believe that some practice needs to be changed.
OB/GYN ultrasound cost
The ultrasound procedure is simple and less expensive. An ultrasound examination can cost anywhere from $200 to $500. In any case, it primarily relies upon the spot you are getting the test and why you are getting tried. The procedure can also be covered by insurance.
3D/4D Ultrasound
What is 3d and 4d Ultrasounds
You can see your unborn child in even more depth and detail during a 3D or 4D ultrasound exam than during a standard 2D ultrasound. You are able to see the actual image of the baby—not just his or her internal organs but also the skin, nose, and tongue—in either 3D or 4D. You will be able to see your baby doing things like kicking and yawning inside the uterus. In the 2D screening, the guardians can see a blurred grayish shade of the image on the screen. This image shows the baby’s internal organs as the device scans through him or her.
Why 3D and 4D sonograms are performed?
3D and 4D sonograms are typically recommended for older mothers and pregnant women who are at risk for complications.
The specialist generally performs 2D ultrasound images to see whether there is any irregularity with the pregnancy. They serve a 2D test to inspect amniotic liquid, baby position, and any inherent handicap.
The fetal anomalies are meticulously examined by 3D and 4D sonograms. They can record congenital fissure and spine issues or examine some other imperfections.
You may perform an Ultrasound for the following purposes:
- determining when your pregnancy is due.
- keeping an eye on your baby’s health.
- confirming that the pregnancy is not an ectopic one, in which the baby grows outside the fallopian tube, but rather a normal one.
- determining the baby’s position and whether or not he is facing the right way.
- Examining the possibility of multiple births.
- determining the fetal and placental sizes.
- determining the baby’s gender.
- assessing the amount of amniotic fluid surrounding the infant.
What is a 3D ultrasound in pregnancy?
In 3D Ultrasound, multiple two-dimensional images from various angles are recorded by the sonographer, who then merges them to produce a three-dimensional image. You will be able to see your baby, for instance, in three dimensions, just like you would with a normal picture on your phone or laptop. His or her face and the entire surface will be visible to you.
What is a 4D ultrasound in pregnancy?
4D Ultrasound is equivalent to 3D Ultrasound, however here you won’t simply see the picture of your child, yet you can see his video. As a result, when you use 4D ultrasound, you will be able to see what your baby is doing right now. As the baby moves or turns, you can clearly see what he or she is doing on the monitor..
The safety of 3D and 4D ultrasounds during pregnancy
Because you will be able to see your little ones, getting a 3D or 4D ultrasound test is a very tempting option. However, medical ultrasound should always be performed, as the American College of Obstetricians and Gynecologists (ACOG) suggests. Both the mother and the baby are protected during the procedure. Although there is no risk, it is best carried out by a trained medical professional only when absolutely necessary.
The use of ultrasound results in the transmission of some tissue heat; accordingly, they make little gas rises in the tissue and body liquids. This warming might hurt your body in the long haul. Additionally, ACOG recommends that pregnant women undergo a 2D ultrasound examination between the ages of 18 and 22.
Difference between 2D, Doppler, 3D, and 4D ultrasounds
Examining the procedure of each type of ultrasound is necessary to distinguish between them:
Ultrasound in 2D: The doctor uses a transducer to send sound waves through your body in this way. At the point when the transducer is squeezed against your skin or put in your vagina, it sends waves that hit the inside organs or liquids and return. The echo produced by this bouncing wave aids in the display of an image on the monitor. The baby’s grayish outline can be seen in this cross-sectional image.
Doppler ultrasound: Doppler ultrasound is a type of ultrasound that helps detect the baby’s heartbeat and blood flow. In order to hear the fetal heartbeat, the radiologist applies a special gel to your abdominal area with a hand-held device.
Ultrasound in 3D: In this strategy, you will see the picture of the child all the more obviously. By recording the internal and external details of the organs from various angles, it creates a three-dimensional image of the baby. You will be able to see the baby’s heart, blood vessels and valves, skin, mouth, or shape on the monitor.
Ultrasound in 4D: 3D and 4D are similar; the main contrast is that by 4D Ultrasound, you will actually want to see the live video of your child. The ultrasound can capture the baby’s line motion, such as when the baby yawns or moves their hands or legs.
How does it work?
In 2D Ultrasound, they send sound waves and reflections from the body to record its reverberation. This echo is interpreted by the transducer to produce an image of the baby.
Similar to 2D ultrasound, 3D ultrasound records the waves from multiple perspectives. Using sophisticated software, the doctors combine multiple images from various angles into a single one. Images are produced using this kind of ultrasound algorithm process, which is also referred to as “surface rendering.” The monitor is shown an accurate representation of the fetus created by this software. The baby’s face and body are depicted in great detail in these stunning photographs.
The procedure for 4D ultrasound is the same, but the images are captured or moved every second. Consequently, the monitor displays video rather than a still image of the baby.
Who takes the exam?
The ultrasound procedure is only performed once for women with a low risk of complications. However, women who are at risk for difficulties or multiple births typically undergo additional testing. There can be many purposes behind getting the test contingent on the trimester. However, 3D and 4D ultrasounds are not required.
What does the exam do?
By recording the sound waves, 3D and 4D ultrasound, like standard 2D ultrasound, also produce images. However, in this instance, a three-dimensional image of the baby is produced. Additionally, a still image will not be altered by a 4D ultrasound; It will be recorded as a video.
How the test is finished?
In the event that you are going for a stomach Ultrasound, the specialist will request that you rests, and the specialist will rub some water-based gel in your gut. The waves are transferred from the transducer into the body and returned by this gel. To create your baby’s image on the screen, the doctor will move the device back and forth.
What to Know About Test Results?
After the test is finished, you will get an image or a video duplicate of the child to bring back home with you. If there is a problem or you need to take some precautions, the doctor will tell you.
Ensure that you play out the test just in a clinical focus by a certified and experienced professional. The medical center is not a substitute for ultrasound at a commercial location.
3D and 4D Ultrasound Side effects
The procedure sometimes slightly heats the tissue, but there are no known side effects. Gas pockets develop within the tissue as a result of the tissue being heated. Therefore, it is best to only carry out the ultrasound procedure when the medical professional requests it. Although there is no evidence to suggest that it harms the mother or the baby in the last two decades, you should avoid it whenever possible.
Between the 26th and 34th weeks of pregnancy, a 3D or 4D ultrasound is recommended by the doctor. Nonetheless, you can likewise get a reasonable picture of the child whenever following 24 weeks of imagining the child.
The benefits of 3D/4D Baby ultrasound
Following are the benefits of the process:
- You will be able to see the live image of your baby’s skin, mouth, or whole surface.
- You can monitor the baby’s size.
- Evaluate his/her movement.
- Confirm the due date.
3D and 4D Ultrasound cost
The procedure is relatively inexpensive; It can cost between Rs 750 and Rs 3000.

